It was just a pedicure. But it could've killed Kim Ealy.
"Whoever thought you could potentially lose your life having a pedicure?" asks Ealy, 44, a Chattanooga woman who contracted methicillin-resistant Staphylococcus aureus (MRSA) from contaminated equipment used during the procedure. "The nail tech cut me and used an implement that had not been sterilized."
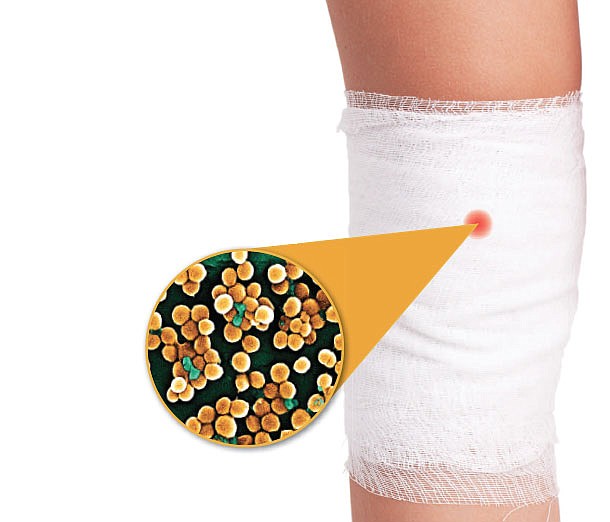
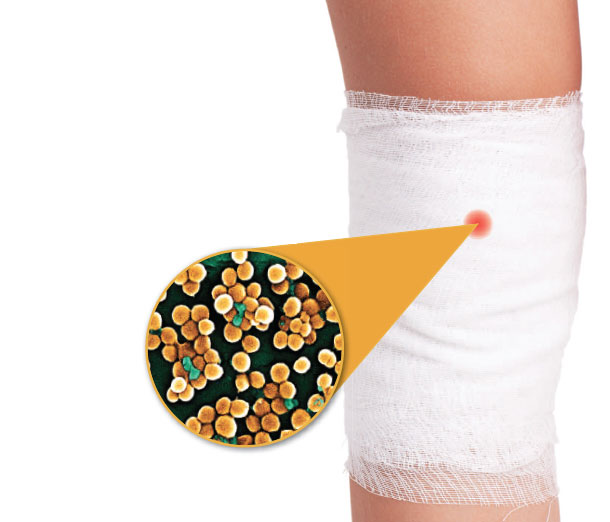
MRSA is a bacteria that is resistant to many antibiotics, according to the Centers for Disease Control and Prevention. Out in the real world, most MRSA involves skin infections, but in medical facilities - where MRSA is often contracted - it can cause life-threatening bloodstream infections, pneumonia and surgical site infections.
MRSA signs and symptomsMost staph skin infections, including MRSA, appear as a bump or infected area on the skin that may be:* Red* Swollen* Painful* Warm to the touch* Full of pus or other drainage* Accompanied by a feverSource: Centers for Disease Control and Prevention
The issue is that MRSA, which first began showing up in the early 1960s, is resistant to the antibiotics normally used to treat staph infections - the penicillins (which includes methicillin) and the cephalosporins.
With decades of research now behind them, scientists and doctors have found new antibiotics to treat MRSA - which is highly contagious through touch - but just saying the name can send people into a panic, thinking the bacteria is a death sentence. While it's nothing to take lightly, MRSA usually is more of a nuisance these days and can be successfully treated in most cases.
Ealy says her case was potentially life-threatening because doctors feared the infection would spread to her bones since the oral antibiotics weren't working. She was treated by three doctors over eight weeks, undergoing X-rays and magnetic resonance imaging to keep a close eye on the infection. Doctors also put her on intravenous antibiotics.
"Once it gets into your bones, that's when it starts spreading quickly and that's how people die from MRSA. I was scared," says the married mother of five children ages 5 to 11. "I had to take a leave of absence from work as I laid in my bed with my toe elevated above my heart six inches."
For two weeks, six hours a day, she was hooked up to the IV, then after a third week with no antibiotics but her toe still elevated, doctors said she was infection free.
More MRSA
While MRSA can be more easily treated these days, the problem is that more cases are showing up.
"I used to see maybe one or two people a year back in the 1980s and '90s with MRSA, but now I sometimes see as many as 10 people a week," says Dr. Mark Anderson, an infectious disease specialist in Chattanooga. "In the late 1990s, a new strain developed out in the community that was different from the hospital strain of MRSA.
"On occasion, it can be scary, but that's very unusual," he says. "But we do see people with dangerous infections. And in recent years, we've seen more pneumonia with MRSA than we used to."
Phyllis Miller, a local gynecologist and former president of the Tennessee Medical Association, says that, though she can't pinpoint the first time she saw a patient with MRSA, she's seeing it with much more frequency over the last five years.
"Many people are aware of MRSA and are very scared of it. They associate it with the more serious illnesses in hospitalized patients and debilitated patients who can get septic and die from it," she says. "The cases we see in the office in healthy people are easier to treat. Most of it responds to sulfa drugs or tetracyclines.
"Also, staph typically causes abscesses, and these respond very well to draining in the office," Miller says. "Medicine is probably better today in treating the more-serious MRSA infections because of the development of some newer and more powerful antibiotics that are given intravenously."
While the CDC says it does not have data showing the total number of people who get MRSA infections in the U.S., it does report that life-threatening cases of MRSA in medical settings are dropping because hospitals and other facilities are taking steps to prevent the spread of the bacteria.
Life-threatening MRSA infections that began in hospitals declined 54 percent between 2005 and 2011, with 30,800 fewer severe infections, according to a CDC study published in the Journal of the American Medical Association Internal Medicine. The study also reported 9,000 fewer deaths in hospital patients in 2011 compared to 2005.
Outside of hospitals, MRSA easily spreads where people are in close contact with one another such as in families, sports teams, day cares and schools. Anderson says most people probably have "colonies" of MRSA somewhere on their skin right now or have had it on them at some point.
"You can almost assume most everybody is colonized with it, though not everybody will start having problems," he says. "It's hard to avoid unless you don't have contact with other human beings. It's safe to say that we all come in contact with it.
"MRSA binds to our skin exceptionally well," he says. "It probably acquired some genetic information from a type of staph called coagulate negative, which is a normal part of our skin that we all have on us."
There's at least 15 to 20 percent of the population colonized with MRSA, Anderson says, "and about 40 percent of people have some type of staph infection on their skin."
But the new strain has features that make it problematic, he says.
"If you get 'colonized' with it (on your skin), you're more likely to start having problems like boils," he says. "I see people all the time who have had multiple episodes of it even though they've taken appropriate antibiotics and had the boils lanced. Antibiotics don't get rid of the colonization, unfortunately."
The second "feature" is that, once you've been treated for a MRSA infection, the bacteria remains in your body, he says. But that doesn't mean you're doomed to get more outbreaks.
It's hard for the lay person to recognize whether or not a small pimple or boil is MRSA. The only way to be certain is to have it lanced and cultured.
"It tends to cause problems in areas of the body which have hair follicles, with the most common areas being on the bottom, upper legs, inner thighs in the groin area and under the arms," Anderson says. "But in the thousands of people I have seen with it in the last 10 to 12 years, I've seen it everywhere - on the face, in the hair, all over."
treatment
If diagnosed with MRSA, it's important to take steps to keep it from spreading. Pus, which often leaks from infected wounds, is laden with MRSA, so keeping the wound covered with bandages is key, the CDC says.
Anyone in close contact with someone infected by MRSA should wash their hands often with soap and water or use an alcohol-based hand rub, especially after changing the bandage or touching the infected wound, the CDC reports. Do not share personal items including towels, washcloths, razors, clothing or uniforms with someone who has MRSA.
Anderson advises his MRSA patients, whether they've had one or multiple breakouts, to use Hibiclens soap, available over the counter at most drug stores. He tells his patients - and everyone in the household, for that matter - to use it twice a week, either in the bath or shower, for two to four months, depending on the severity of the MRSA.
"It can help get rid of the colonizations," he says. "I tend to have people use it a little bit longer than medical literature suggests it should be done. I usually follow literature close, but I've seen so much MRSA and so many recurrences that I think the Hibiclens soap should be used longer, and it's something safe for long-term use."
Maura Lambert was introduced to MRSA several years ago when her teenage son contracted it at a summer camp.
"The first time he got it was upon returning from camp," she says. "He had a little bump on his face, and I thought it was his first pimple. It wasn't. We left for Florida and, by the time we returned home, he had a fever. I got him to the doctor, and after some serious antibiotics, it healed."
Two years later at football camp, her son's MRSA resurfaced on his foot, she says
Their doctor "knew with one look what it was," Lambert says, "and prescribed an antibiotic and sent us home after drawing a red circle around the reddened area with instructions to come back if the hard red swelling went beyond the circle."
It did.
"She admitted him to the hospital. He was put on intravenous antibiotic, and there was no change. Day two, no change."
Finally, the doctor lanced the boil on his foot. "It was only then that it healed."
And yes, she was terrified.
"I'll never forget it," she says. "I don't blame the camp. I believe the situation with over-prescribed antibiotics and people misusing them is what is causing this problem."
Some disease-causing bacteria worldwide have developed resistance to antibiotics after being exposed to them time and time again. "Although experts are working to develop new antibiotics and other treatments to keep pace with antibiotic-resistant strains of bacteria, infectious organisms can adapt quickly," reports the Mayo Clinic. "Antibiotic-resistant bacteria will continue to be a global health concern and using antibiotics wisely is important for preventing their spread."
Gynecologist Miller suspects that overuse of antibiotics is the reason she's seeing more MRSA.
"Staph has been around for a very long time, but the methicillin-resistant staph has evolved," she says. "Germs are very smart and, as they are exposed to antibiotics, they are good at mutating to a form that is resistant."
Meanwhile, for most of those diagnosed with MRSA, if you're feeling OK, if the infected area is properly covered and you're doing proper hand hygiene after touching it, it's OK to go back to work, school, day care and other daily activities, says Anderson.
The best case of defense is to wash your hands often, says Anderson, who practices what he preaches, washing his hands with Hibiclens soap 40 to 100 times a day.
Ealy says she's taking steps to make sure she doesn't get it again.
"I'm definitely more aware of MRSA now and I'm very cautious with open wounds or scrapes, and I always wash my hands with bacterial soap and use sanitizers," she says.
Contact Karen Nazor Hill at khill@timesfreepress.com or 423-757-6396.