The ongoing debate in Washington, D.C., over the future of Obamacare may determine how many people have health insurance, but it won't necessarily change how health care is delivered or alter the way Chattanoogans deal with the single biggest cause of death.
That may require a new approach to fighting cancer, which is second to heart disease as the top killer among all Americans. The No. 1 cancer in Chattanooga is lung cancer, and experts say the key to limiting deaths from lung cancer is to target those susceptible to the disease and provide easier and more widespread early detection and treatment.
"If we find out who those people are that are at high risk, capture them as they are coming into the hospital or doctor's offices and then proactively work to engage them in early screening, we have a great opportunity to lower the number of deaths from lung cancer in our community," said Dr. Rob Headrick, a specialist in thoracic and lung care who is pushing for a new population-management approach to treating the disease.
The five-year survival rate for lung cancer has remained stubbornly low, at only about 18 percent, for most of the past 40 years, Headrick said. But if detected in early stages or before tumors develop and grow, the 10-year lung cancer survival rate is 90 percent.
"We're approaching the disease the wrong way and we are spending a lot of money without getting a major impact from it," Headrick said.
To better target those susceptible to lung cancer and provide better education and training for such people, CHI Memorial has invested in pioneering software to help identify those at risk and those who may have shown signs of potentially developing cancer.
CHI Memorial was the first hospital in the country to buy software developed by MedMyne that uses natural language processing to search medical records and identify the most at-risk population. The MedMyne software allows Memorial to mine data from imaging tests, physician visits and hospitalizations.
"Every cancer we can catch early and cure is a gift," said Memorial CEO Larry Schumacher, a trained nurse. "So doing this is just the right thing to do."
Based upon clinical and population studies, Headrick estimates some 30,000 people among the nearly 550,000 residents in metropolitan Chattanooga are most at risk for lung cancer. They include those 55 and older who have smoked at least 30 packs of cigarettes a year in the past 15 years, those who may have been exposed to radon or asbestos, and those with a family or personal history of cancer.
"Our approach in the past to try to detect someone who might have lung cancer was to target the entire population," Headrick said. "Well, that's wasteful and a lot of people don't need to hear about it and genetically or socially they are never going to develop lung cancer."
Headrick was pitching the idea of better population management of the disease in Schumacher's first week as Memorial's CEO in January 2016. Schumacher agreed to make the technology investment and is now working to develop easier and more effective ways to easily screen those at risk.
"Is this data in the medical record or the imaging that may have been done on someone? Yes," Schumacher said. "But is it easily gathered if you are looking at a population of people who are at high risk? The answer is no. That is why this software is so innovative, because it helps us to identify those at risks and get that information to the primary care physicians."
Convincing more people to get tested for lung cancer and then getting those who turn up positive into treatment quickly is key to successful treatment, doctors say.
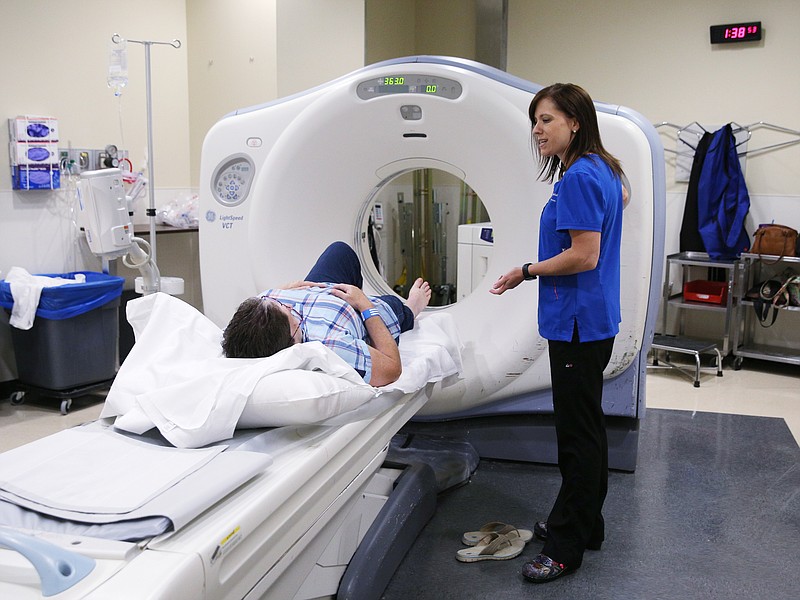
The tools to detect and treat cancer continue to improve, allowing for easier screening and less-invasive surgeries. CT scans, which improved on the less precise X-rays of the past, are better able detect small cancers while they are still tiny and easier to treat.
"CT screening is a huge deal, a major deal," Dr. Krishnendu Bhadra, an interventional pulmonologist at CHI Memorial, told the Times Free Press last year. "Lung cancer kills more people than breast, colon and prostate cancer combined."
Radiation therapy also has improved with new techniques to better target a tumor's exact location and use multiple beams of radiation to reduce the number of treatments required. That usually reduces the number of visits for radiation therapy by more than 80 percent from what was required a decade or more ago.
Surgical procedures also are far less invasive than in the past. When Headrick began as a lung surgeon, cancer removal surgeries required spreading the ribs and making a large incision, so the average length of a hospital stay was more than a week. Surgeons now can make a small incision in the side of the chest and a patient can go home the next day.
But corrective surgery is usually effective only if the cancer is caught before it is stage 3 or 4 and has spread to other parts of the body.
Smokers, war veterans or others with family history of the disease sometimes are reluctant to seek testing, even though the early-stage lung screening is paid for under Medicare and commercial insurance plans for those at risk, Headrick said.
"Smokers don't want to be lectured to and sometimes they are reluctant to get tested because they just don't want to know what they fear may be the case," he said. "But the reality is that most smokers don't get lung cancer, even though they have a higher propensity for the disease, and if it is caught early this is no longer a fatal disease."
Doctors hope the MedMyne software will help identify those most at risk and make lung screenings easier to schedule or perform in conjunction with other health care services. Memorial is looking at ways to possibly offer mobile screenings at worksites or local organizations to take the technology directly to the people.
"We have to make screenings convenient for the patient and not require that they take time off of work or spend a lot time at the doctor's office or hospital," Headrick said.
Studies at the Mayo Clinic and elsewhere indicate that often once smokers realize they don't have cancer - or get surgery to treat early stage cancers - they are more apt to change their behavior and less likely to get the fatal versions of the disease.
"Regardless of what happens in Washington over health care reform, the honest answer is that whatever Congress decides is not going to change how many people die with lung cancer in Chattanooga," Headrick recently told the Chattanooga Rotary Club.
"But with what we are doing, I think in 10 years we can truly change lung cancer and its impact on Chattanooga. Lung cancer is curable and we have the talent here and the ability to truly be a national model for a new and better approach to health care."
Contact staff writer Dave Flessner at dflessner@timesfreepress.com or at 423-757-6340.
Targeted population for early lung cancer detection
› 55- to 75-year-olds who smoked at least 30 packs of cigarettes a year in the past 15 years› Family history of cancer› Those with other types of cancer
Why Chattanooga has higher lung cancer
› Higher rate of smoking. More than one in five adults smoke and nearly half of all adults have smoked sometime in their lives.› Higher rates of radon, a radioactive gas found in igneous rock, soil and sometimes well water. Hamilton County has moderate potential and Bradley, Rhea and McMinn counties have the highest potential.› Asbestos and air pollutants. Because of Chattanooga’s concentration of heavy industry, its air quality was rated as the worst in the country in 1969. Air quality has improved since, but higher levels among those who have been in the military or worked in factories can contribute to more lung problems.› Lower education and socioeconomic background, which tends to lead to more unhealthy behaviors.Source: Hamilton County Department of Health, Tennessee Department of Health