DID YOU KNOW?• Some 36 million Americans -- roughly 10 percent -- suffer from migraine headaches.• The majority of migraine sufferers are women.• U.S. employers lose more than $13 billion annually as a result of 113 million lost workdays due to headaches or migraine headaches.• Migraine medications do not cure migraines; they treat symptoms.Sources: Dr. Jimmy Waldrop, healthline.com
Heather Crowe has suffered from migraine headaches for 30 years.
Sharp, stabbing, incapacitating pain in her head -- usually preceded by nausea and blurred vision, she says -- that forced her to lay down in a darkened room and wait it out.
The first one was in junior high school, and they escalated in pain and recurrences until violent headaches were occurring five to seven days each week when she was an adult. Although she took two medications, they didn't always control the pain; migraines controlled her life.
"Sometimes the medication would work so that I could still function, but most of the time I had to go to bed where it was dark and quiet," the 41-year-old recalls.
The mother of twins says her sons just knew mom "had to go to bed and I couldn't do anything. We didn't make a lot of plans. It was a day-to-day thing."
A migraine headache is a neurological disease that involves a headache commonly described as intense throbbing or pulsating pain in one area of the head. The pain may be accompanied by extreme sensitivity to light and sound, nausea and vomiting.
"Nothing would work and I was miserable," she says of treatments prescribed by her general practitioner and her gynecologist. "I was ready to try anything."
So in December, Crowe became the first person to undergo surgical nerve decompression for the relief of migraine headaches in Chattanooga.
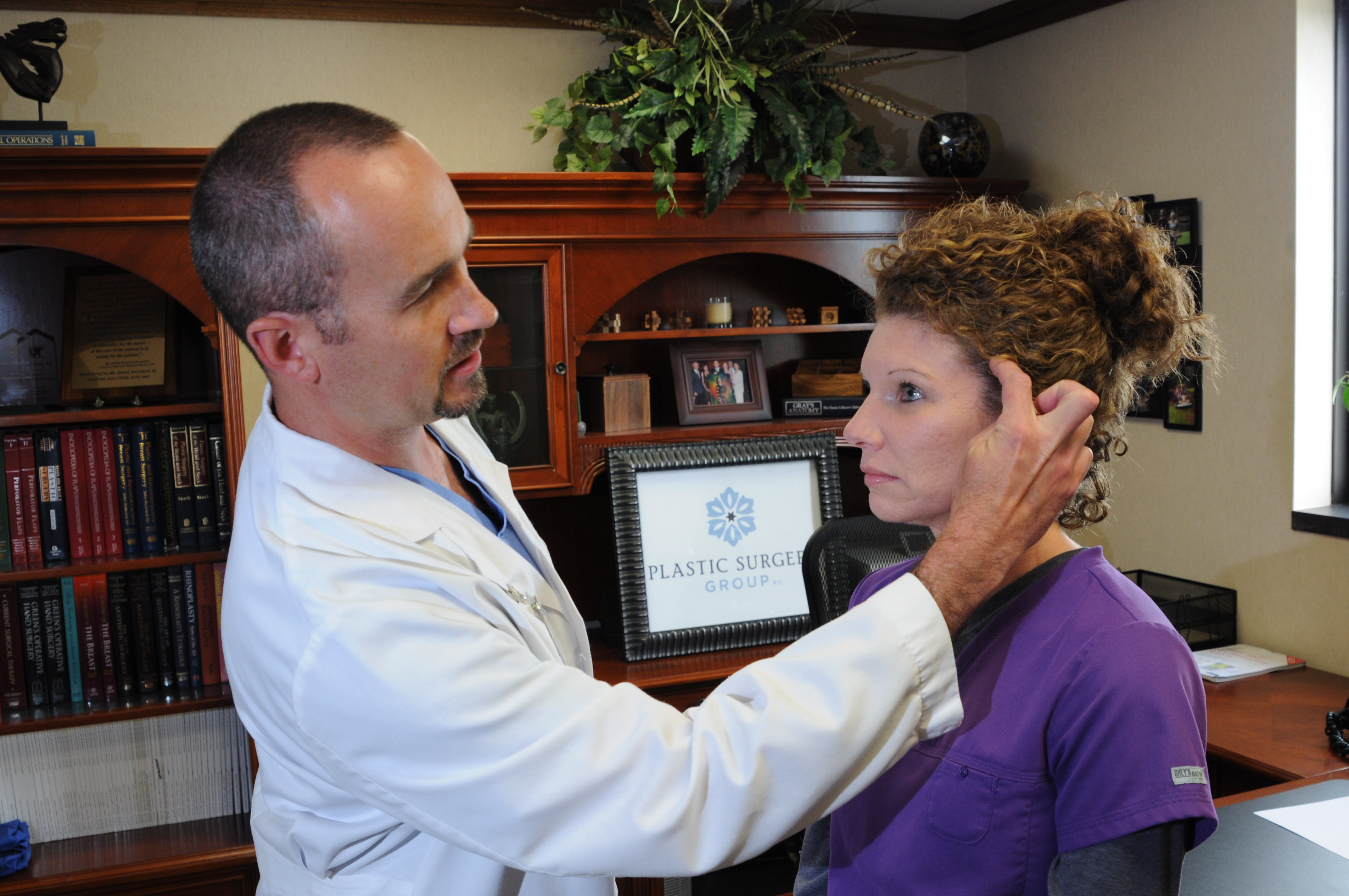
The outpatient surgery was performed at Erlanger hospital by Dr. Jimmy Waldrop of the Plastic Surgery Group, the first surgeon to bring the procedure to Chattanooga. While the surgery has been performed successfully by surgeons in other parts of the country, Waldrop is the only area physician to date offering it. Crowe is a medical assistant in the Plastic Surgery Group's office, so Waldrop is familiar with her case.
Crowe says she has had four headaches in the six months since she had surgery -- a tremendous improvement over her previous average.
THE PROCEDURE
Some Internet websites have dubbed the procedure the "brow lift for migraine relief," due to its similarity to a brow/forehead facelift; both surgeries involve short incisions made in the scalp line at the top of the temple.
But Waldrop pans that comparison, pointing out that this procedure is surgical treatment for migraine headaches while a brow lift is a cosmetic procedure to tighten and lift sagging skin on the forehead.
"Nerve decompression is a minimally invasive procedure performed by small incisions behind the hairline: five in the front, one in back," Waldrop describes. "The goal is to identify trigger points, which are in the temple and back of the head. Once identified, the goal is to decompress those nerves involved. Decompression involves cutting them away from what they are attached to, freeing them up from whatever is pressing on them. The irritation to those nerves causes migraines."
While Crowe is Waldrop's only patient to have the surgery so far, he says he has received eight patient referrals from local neurologists for consultations. Dr. Ravi Chander is one of them, but the neurologist said in a statement through his office that he felt it was too early to give a fair, accurate evaluation of the procedure at this early point.
While some surgeons express skepticism that the procedure actually works, studies have shown that a signficant number of migraine sufferers do find relief after surgery.
In a study at Case Western Reserve University, patients were divided into two groups, one had the surgery, the other had a sham procedure in which they were put under general anesthesia, an incision was made and the nerve was exposed but not completely decompressed. There was a 57 percent cure rate -- complete elimination of migraines -- in the surgery group versus a 4 percent cure rate in the sham surgery group, the study showed.
Waldrop says he has seen studies that show 90 percent of patients experienced significant improvement in symptoms and 60 percent became headache-free.
ELIGIBLE CANDIDATES
Waldrop lists three criteria for the ideal candidate.
• The candidate must have had a neurologist or experienced physician give a medical diagnosis of migraines -- an important distinction, he explains, from tension or cluster headaches.
• The candidate must have tried and failed medical management with medications.
• The candidate has severe, frequent headaches with identifiable trigger points.
Waldrop says the cost of the surgery will depend on the number of trigger points treated; the higher the trigger points, the higher the expense because the surgical procedure takes longer. The physician noted that in states where the surgery has already been performed, it has "generally been covered by insurance."
"Since we have only performed one migraine headache surgery and are still working with the insurance company and hospital systems, there isn't enough available information to accurately determine a price range for migraine headache surgery," says Andre Charitat, communications specialist for the Plastic Surgery Group.
RECOVERY
Post-op, a patient will require about four weeks until resuming regular activity, says Waldrop.
"It's common to have a headache for about a week after surgery. Then, depending on how the individual feels, they can generally stop taking their usual migraine medications," says the surgeon.
"Studies that followed patients for up to five years found that where the patients were in a year was likely their final result from the surgery. If there haven't been any headaches in a year, then you probably won't have more. If you are still having headaches, then that treatment wasn't successful."
After two months, Crowe says she was able to get off her medications.
"Without a doubt, this procedure gave me life back. We plan stuff now. My boys and my husband think I am completely different. I'm not in the bed all the time," she says.
Contact Susan Pierce at spierce@timesfreepress.com or s423-757-6284.