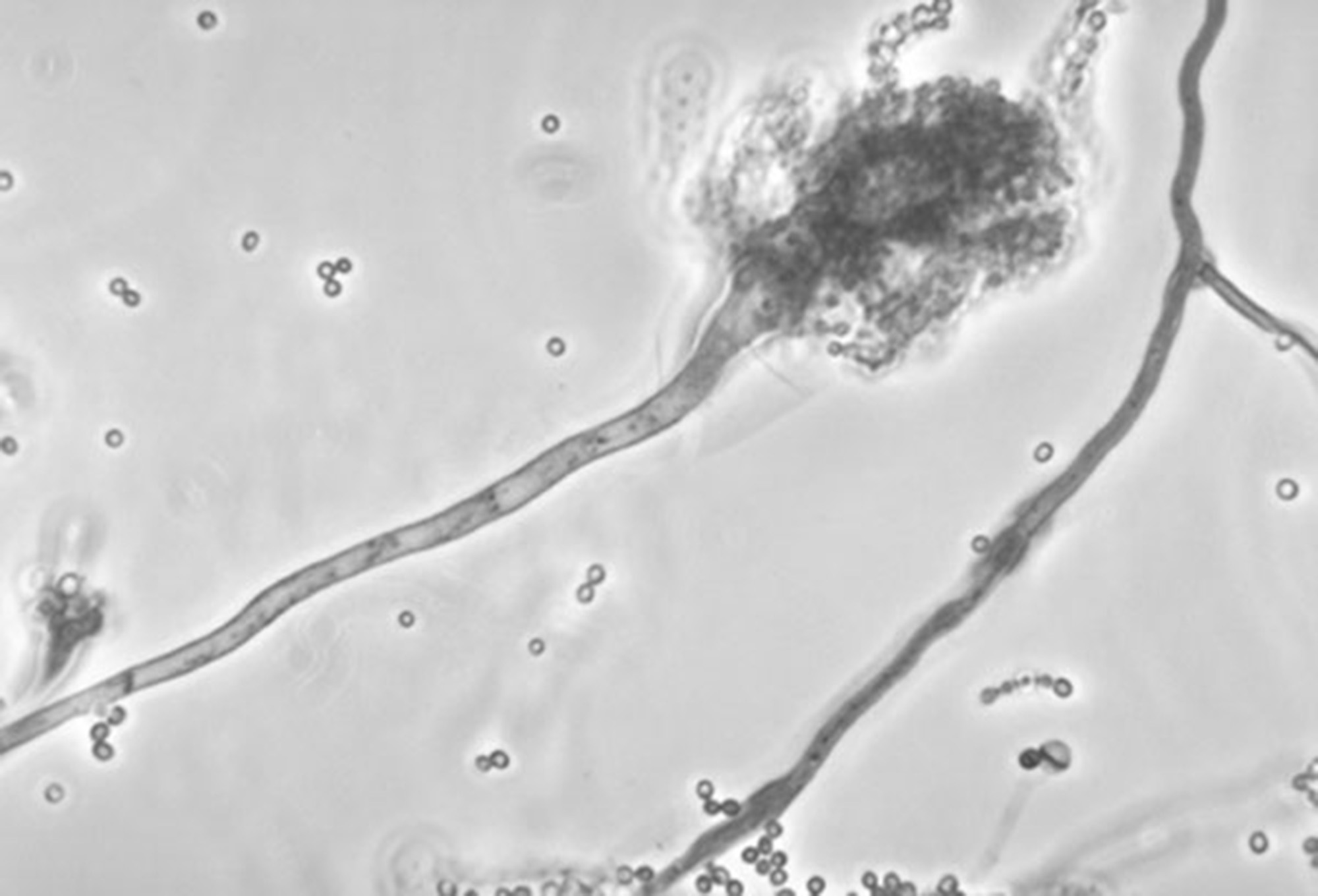
 This undated photo made available by the Centers for Disease Control and Prevention shows a branch of the fungus Aspergillus fumigatus. The fungus can also cause skin infections if it enters a break in the skin. The meningitis outbreak is linked to the fungus being accidentally injected into people as a contaminant in steroid treatments. It's not clear how the fungus got into the medicine.
This undated photo made available by the Centers for Disease Control and Prevention shows a branch of the fungus Aspergillus fumigatus. The fungus can also cause skin infections if it enters a break in the skin. The meningitis outbreak is linked to the fungus being accidentally injected into people as a contaminant in steroid treatments. It's not clear how the fungus got into the medicine.NASHVILLE - Members of Tennessee's Board of Pharmacy recently revoked the license of the Massachusetts pharmacy linked to a deadly meningitis outbreak, but a review by The Tennessean shows the board has been lenient on compounding pharmacies in this state accused of violations.
The Tennessean found that a letter of warning was the typical response to infractions, including sterility problems, expired drugs and unlicensed pharmacists.
The review also found the board keeps secret the names of pharmacists who are sent the letters.
Tennessee has not adopted model regulations for sterile compounding. It also does not require a separate license for sterile compounding, so the Health Department doesn't know how many pharmacists do it.
And the board has just five inspectors to regulate more than 10,000 pharmacists.
As the board prepares to meet this week, no new regulations for sterile compounders in Tennessee are planned.
Since 2007, the board has heard at least 13 complaints related to compounding. In six cases, the board sent letters of warning or letters of instruction to the pharmacist. Four cases either were either dismissed or the board took no action. One case resulted in a fine, and two cases resulted in formal cease-and-desist letters.
The most common compounding complaint relates to pharmacists operating as a manufacturer by preparing medications without a doctor's prescription, which the law requires. The New England Compounding Center in Massachusetts, which produced the contaminated steroids that have caused a deadly fungal meningitis outbreak, was doing the same thing by preparing the steroids in bulk.
Pharmacists who engage in this practice are supposed to be licensed as manufacturers, in which case they are subject to federal oversight.
Tennessee's pharmacy board also has approved licenses for pharmacists with histories of disciplinary action related to compounding practices in other states.
In 2004, the U.S. Pharmacopeia developed model standards for sterile compounding. Those standards have been adopted in 18 states, according to the National Association of Pharmacy Boards
The Tennessee pharmacy board already has regulations related to sterile product preparation, but the state has not incorporated the model regulations.
The Tennessee Pharmacists Association, the state professional association of pharmacists, has convened an advisory committee to study rules and regulations related to compounding after the New England Compounding Center situation. One member of the panel is Nashville pharmacist John Hollis, who was disciplined in 2009 by the board for preparing medications without a prescription for specific patients. He said the committee probably would recommend the adoption of the model regulations.
Tennessee Board of Pharmacy member Joyce McDaniel, who is the board's designated consumer advocate and the only member who is not a pharmacist, said it was appropriate to consider new regulations after the outbreak.
"I believe the board should consider reviewing all rules, especially where it concerns sterile compounding and manufacturing," McDaniel said.