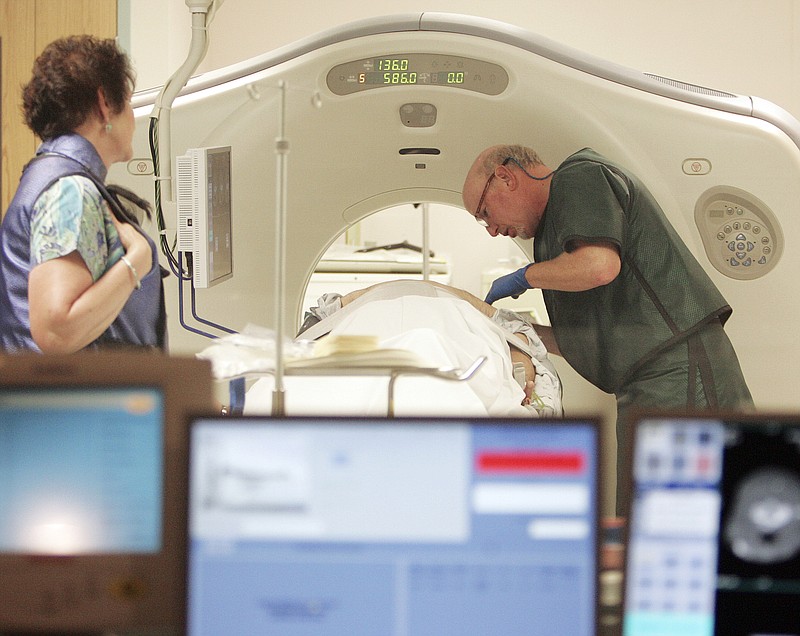
Jenny White discovered her lung cancer because of a dirty bathroom.
"There was mold on the ceiling of the shower," she said, "so I started spraying bleach on it."
She also had been cleaning the walls with an ammonia solution, and the combination forms toxic fumes. She started coughing and rushed to her doctor.
In a chest X-ray, her physician discovered a small nodule.
Uneven funding
Dollars for cancer research, per fatality:› Lung cancer: $1,680› Colorectal cancer: $6,344› Prostate cancer: $12,644› Breast cancer: $25,118
"I had never smoked and there was no one in my home who had ever smoked, so I was sure that it was not lung cancer," she said in an interview Friday.
But after two years of monitoring, the tumor grew 30 percent. A biopsy confirmed it was lung cancer.
White was fortunate - the cancer was caught in the early stages and removed surgically. She has been cancer-free now for five years.
Today she shares her story for a reason: She realized there "were not enough survivors to tell the story."
The Nashville woman is now the state chapter director for the Tennessee Lung Cancer Alliance.
Lung cancer is the deadliest cancer for women - more so than breast, ovarian and cervical cancer combined. While 90 percent of breast cancer patients are alive five years after their cancer is detected, only 20 percent of lung cancer patients survive that long.
Fewer than 20 percent of lung cancer patients are lucky enough to have their tumors discovered at Stage 1.
Compared to breast cancer, where mammograms have long been accepted as a way to detect the disease early, there has been no comparable tool for lung cancer.
"There hasn't been an approved screening until recently," said Dr. Pamela Sud, a lung cancer specialist at CHI Memorial hospital. "When a patient would come in, they might have bronchitis or COPD [chronic obstructive pulmonary disease], but unless they had an unexplained weight loss or were coughing up blood, we never knew they might have cancer."
Even when late detection was not fatal, lung cancer patients had to endure a grueling regimen of radiation and chemotherapy.
Screening got a big boost two years ago, when a panel of medical experts recommended women aged 55 or older who have been regular smokers get a CT scan of their lungs every year.
Those scans are now covered by Medicare and most private health insurance as well, Sud said. For women under age 55, or who have not been regular smokers, there is no recommended screening, but they can ask their doctors for a chest X-ray or get a CT scan at a private diagnostic lab, said Dr. Derek Holland, medical director for the Sarah Cannon Cancer Center at Parkridge Medical Center.
That would be recommended for any woman who has been regularly exposed to secondhand smoke as well, Holland said, since some 20 percent of the women who develop lung cancer have never smoked.
On another front, researchers are making slow progress in curing lung cancer.
"There are really exciting things happening," Holland said. "We see advances every year."
He pointed to the increased use of targeted therapies, "designer drugs that instead of killing everything, target one particular protein." Other new drugs either rev up your immune system to better allow it to fight cancer or take the camouflage off of cancer cells that allow them to hide from the immune system.
Unfortunately, after declines for many years, the percentage of young women who smoke has increased in recent years. There is a direct link between that smoking and lung cancer -"85 to 95 percent of lung cancers are related to smoking," Sud said.
That link often seems to give lung cancer a stigma when compared to breast cancer, Holland said.
"People say they did it to themselves, they smoked all their life and this is what they got," he said. "That plays into the discrepancies in funding for the two types of cancers."
According to the nonprofit LUNGevity Foundation, the ratio of federal funding to cancer deaths is $1,680 for lung cancer, $25,118 for breast cancer, $12,644 for prostate cancer and $6,344 for colorectal cancer.
Lung Cancer Alliance director White said that stigma is unfair.
"Only about 20 percent of lung cancer patients are actively smoking," she said. "Sixty percent have stopped smoking and then are diagnosed with cancer 10, 15, 20 years later."
White hopes to lobby the federal government to provide more money for lung cancer research. But she needs more survivors to help her out.
"Two years ago, we participated in a LUNGevity walk in Nashville and I got a green T-shirt as a survivor, but I didn't see any other green T-shirts," she said. "I went up to the organizers and asked how many green shirts they had given out. They said there were only three, the other folks were too ill to participate."
With the new screening guidelines, White hopes more lung cancers will be discovered earlier.
"And with the use of new targeted chemo treatments, that's going to be creating more survivors," she said. "So hopefully there will be a day when we will be strong in numbers and the awareness will be there."
Contact reporter Steve Johnson at sjohnson@timesfreepress.com, 423-757-6673, on Twitter @stevejohnsonTFP and on Facebook at stevejohnsonTFP.