By the numbers
› 120,000 men, women and children await lifesaving organ transplants. › Every 10 minutes another person is added to the national transplant waiting list. › 8,000 deaths occur every year in the U.S. because organs are not donated in time. › 82 percent of patients waiting are in need of a kidney. Source: www.donatelife.net
How to help
GoFundMe - Hope for Ahmya
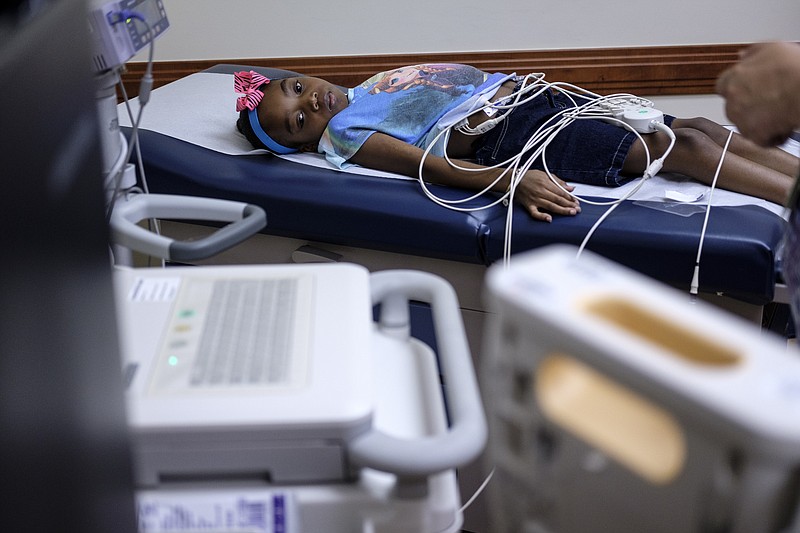
NASHVILLE - By the time Darnima Calloway and her daughter Ahmya got the good news, they had spent two and a half hours bouncing from a waiting room to an EKG lab, to a visit with a nurse to check Ahmya's weight, a blood test, another examination room, another waiting room, and yet another examination room at Vanderbilt's Monroe Carell Jr. Children's Hospital on Thursday.
But it was worth the wait. All of the tests doctors had done to check on 13-year-old Ahmya's (ah-MY-a's) new heart and kidney transplant were good, and she could go home to Chattanooga, needing only to return once a week for the next few weeks.
It was the news Darnima had been waiting for. After years of making the two-hours-plus bus ride to Vanderbilt for kidney dialysis three times every week, months when her daughter lay in a hospital bed, hoping doctors could find a heart and kidney donor before her failing heart gave out, and now eight weeks after the difficult but successful dual heart and kidney transplant, she could pack her bags and head home from the motel room where she had spent much of the past five months.
But instead of celebrating, Darnima was on the phone, trying to raise money to pay this month's rent and stave off an eviction notice until she can get back to her evening job at a copying service in Chattanooga.
Ever since Ahmya was born, Darnima has struggled to overcome one obstacle after another to meet her daughter's medical needs. She doesn't seem upset about this latest setback. When you've kept your child alive for 13 years despite bad kidneys and a failing heart, an eviction notice seems manageable.
* * *
Ahmya's kidneys have been weak from the time she was born, according to Dr. Kathy Jabs, an associate professor of pediatrics and a kidney specialist at Vanderbilt who has treated her since birth.
"The weak heart is a consequence of the kidney disease," she said.
When she first met Ahmya, Jabs was traveling regularly to Chattanooga from Vanderbilt to work at a clinic for kidney patients. In her early years, Ahmya had kidney dialysis on a machine at home. Ahmya was small - at 13, she still weighs only 50 pounds - but despite her weak kidneys, she was able to run around the yard and terrorize her brothers, her mom said.
In December 2012, her doctors decided Ahmya's home dialysis was not working. She needed a higher level of dialysis not available in Chattanooga, so Ahmya dropped out of school and the three-times-weekly trips to Nashville began. After her car broke down, Darnima took a van provided by TennCare, the state's Medicaid plan, on the long trip from Chattanooga to Nashville.
Ahmya had just started the fourth grade at the time, but her education was limited to twice-a-week home schooling visits from a teacher. And there was a social cost - Ahmya lost touch with her classroom friends.
The thrice-weekly trips were a grind. Darnima's other children complained: "You're always gone with her."
But in February, things got worse.
Mother and daughter were on a routine visit to Nashville when they got disturbing news: Ahmya's heart was weakening. The doctors had detected an irregular heartbeat and decided she could no longer remain at home. She needed to stay at Vanderbilt.
Her mother had only packed for a one-day visit. "I had to go out and buy pajamas, socks, toothpaste," Darnima said.
Ahmya became a full-time patient at Vanderbilt. She needed a heart and a kidney, but there were no donors immediately available. Currently, 2,500 people are waiting for a kidney transplant in Tennessee and more than 100 are hoping for a heart donor. Fortunately for Ahmya, if a donor is in good enough health to donate a heart, their kidney is generally also in good enough condition to be used in a joint heart-kidney transplant.
But for the time, Ahmya could only wait, and her doctors were worried.
"There were signs her heart was declining even more," Darnima recalled. "The doctors said she didn't have much time."
Weeks turned into months, but finally, in early May, the word came - a donor had been found.
Doctors scheduled her surgery for the following day. It would be the first time a doctor in Tennessee had performed a dual heart and kidney transplant in a child, one of only 37 in the entire United States.
When a heart transplant was first performed in 1967 by South African Dr. Christiaan Barnard, the world was astonished. Other than the brain, the heart is the most important organ in the body - without its constant pulsing, there would be no life-giving blood coursing through the arteries to bring oxygen to cells throughout the body. The heart seemed to symbolize life itself, and doctors' ability to replace an ailing one seemed to signal a new era in medical care when an out-of-control body could be tamed and tinkered with, not unlike how a mechanic would swap out the engine in a car.
Kidney transplants were first performed in the 1950s, using a second kidney donated by someone who was still living, but it was not until anti-rejection drugs were developed in the early 1960s that transplants from a donor who had died were feasible.
The heart is the hardest part, because speed is essential, said Dr. Bret Mettler, the head of pediatric transplants at Vanderbilt Hospital, and the doctor who performs all of the heart transplants at the Children's Hospital, including Ahmya's.
Shortly after he got word that a donor had been found, Mettler was on a private jet heading to the donor's hospital. After checking that the heart was in good shape, it was removed, placed in a carrying case, and Mettler headed back to Nashville.
In the meantime, around noon, Ahmya had been taken to the operating room, where Dr. Karla Christian was standing by, ready to remove her heart once she got the word that Mettler was getting close to the hospital.
"To do a heart transplant takes two surgeons," Mettler said. "One to go retrieve the donor heart, and one to start the operation so when the donor organ arrives, it can be implanted as quickly as possible."
Mettler said he normally calls the operating room when he gets to the hospital parking lot.
"The goal is, as we walk into the door of the operating room, the native heart is taken out and the patient is on a heart-lung machine and waiting for us to put the new organ in their chest," Mettler said.
Removing the heart and replacing it is a relatively straight-forward process, Mettler said. There are five connections that need to be cut, and those same five connections need to be sewed together when the new heart is in place.
When things work as planned - and they did with Ahmya - the entire process is completed in four hours.
"And that includes everything," Mettler said. "Taking out the donor heart, transportation time, and sewing the new heart back in."
Late that evening, Ahmya was wheeled into the Intensive Care Unit for recovery. The hospital staff worked to stabilize her condition, looking for any sign of infection.
Early the next morning, Ahmya was back in the operating room, where one of the donor's kidneys was attached. Because kidneys can be kept outside the body for 24-30 hours, the kidney operation can be delayed long enough for doctors to be certain that the heart transplant has been successful, Mettler said. Since the body needs only one of its two kidneys, only one is typically transplanted, leaving the other to be used by another transplant patient.
Ahmya was sedated for several days while the incisions from the operation healed. At first, she could only sit in a rocking chair, but now she moves with no sign that she has undergone serious surgery.
She needs eight different types of medication, but the most important are the anti-rejection drugs.
"The body says to the heart, 'You don't belong here, but I'm not going to react a lot because the drugs make me not react a lot,'" Jabs said. "But if you didn't take the medications, the body could fight you off."
Almost immediately, her mom noticed a change in her behavior. "She's perkier," Darnima said.
After being discharged from the hospital, for the next month Darnima and Ahmya stayed in their motel near the hospital. Because Darnima has no car, she has to walk to nearby restaurants to buy meals. Unfortunately, Ahmya has developed a love of Chinese food and the nearest restaurant is a tiring walk on a hot day.
On Thursday, mother and daughter were at the hospital for a 9 a.m. appointment.
Things are almost routine now. First, a blood test, but the nurse always sweetens the deal with a treat.
"We have a love-hate relationship," she said with a laugh. Then an EKG, then a visit from a doctor. He pressed Ahmya's chest and stomach. "Any pain?" Ahmya shook her head, No.
Then it was back to the clinic waiting room, filled with a dozen other children, some energetic, some obviously ill, before yet another examination room, this time for her kidneys.
Jabs asked what she is eating, whether she felt any pain and then asked her to climb up on the table for a closer look.
Everything was fine. And then, the words Ahmya and Darnima have waited so many years to hear: "You only need to come back once a week now, you can go home. We'll do that for a while and then reduce it to once every other week and then once every six months and once every year."
If Ahmya was happy, she didn't show it, engrossed in a photo on Snapchat. But her mother did.
"There is an end in sight," Darnima said. "There is a lot of stuff that she couldn't do. For example, we couldn't take a family vacation."
She wasn't sure she would get the good news Thursday so she hadn't even packed.
This fall, Ahmya will enter the seventh grade at Ooltewah High School. She's looking forward to it, but the transition may not be easy. She has been out of the classroom for three years now and her shyness could be a problem. She spends much of her time on her iPhone and iPad. When she was in the hospital, she often communicated with her nurses by text messages, sending them notes like "I feel like I'm going to throw up" instead of talking to them in person.
She's a "night owl" her mom said, not accustomed to getting up early to get ready for school.
And then Darnima revealed something else. She had been feeling tired, understandable given how hard she was working to deal with her daughter's medical condition. But when doctors ran tests in September 2014, they discovered she is suffering from a mild form of leukemia. It is not life-threatening, but she needs to take medication regularly.
Had she been taking her pills? Before her mom could answer, Ahmya shook her head, no. There hasn't been time to get the prescription filled, Darnima said.
But now she has time.
As for Ahmya, despite everything, she seems to like hospitals.
"She wants to be a nurse when she grows up," Darnima said. "She wants to work at Vanderbilt with babies."
Contact staff writer Steve Johnson at 423-757-6673, sjohnson@timesfreepress.com, on Twitter @stevejohnsonTFP and on Facebook, www.facebook.com/noogahealth.