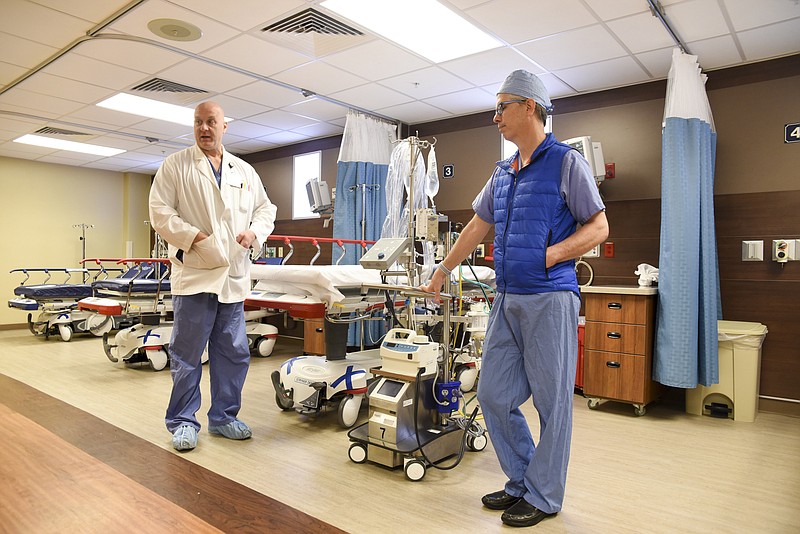
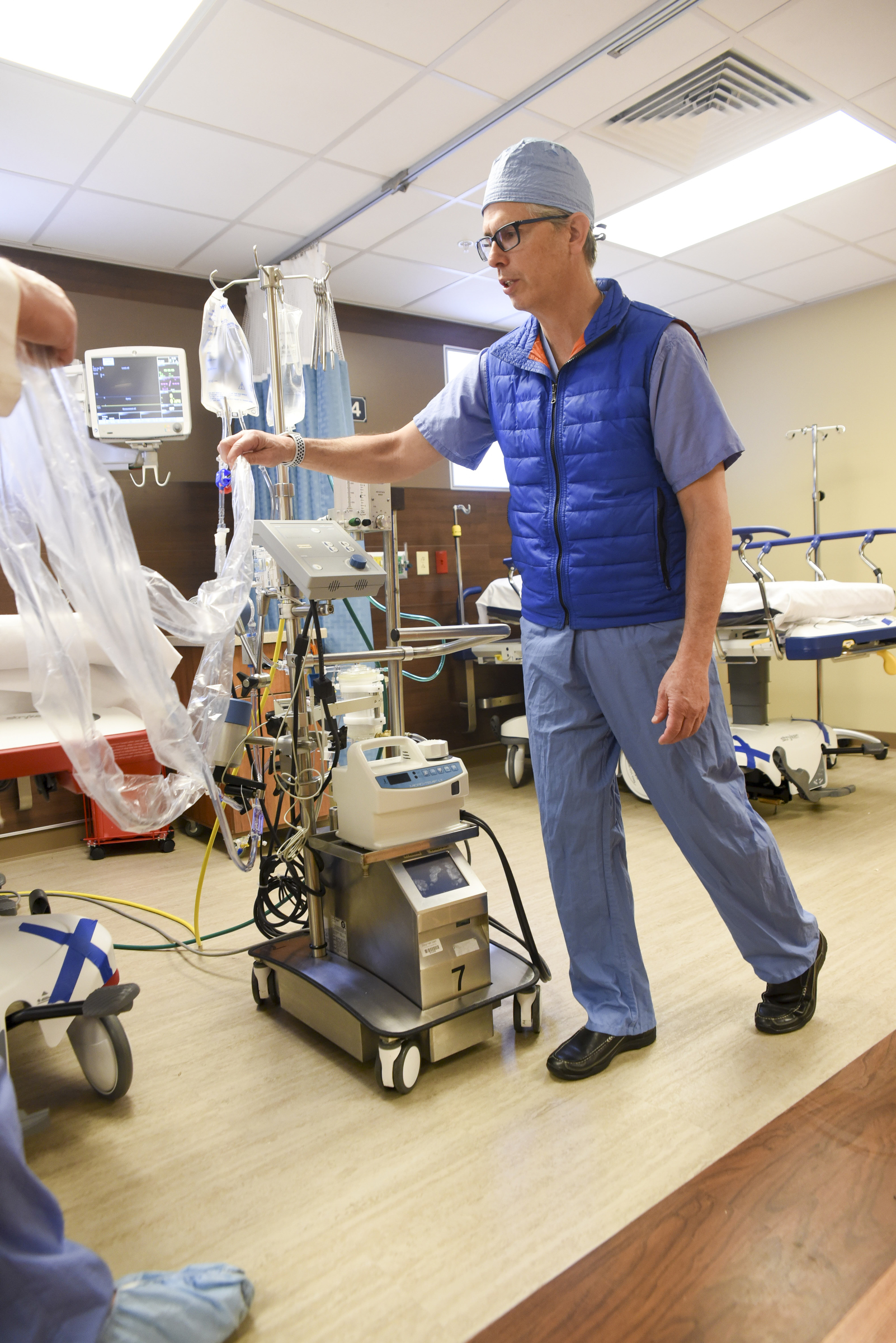
The burden of this year's influenza season - which struck the Chattanooga region, like most of the nation, early and hard - is evident in its toll on the health care system.
Nationwide, hospitalization rates for the flu are the highest since the U.S. Centers for Disease Control and Prevention began collecting such data in 2003.
Although most people recover from the virus on their own or with basic care, some develop serious complications that land them in the hospital. Older adults, children and people with chronic medical conditions are most vulnerable to these effects.
"We were much busier and stressed dealing with a lot of the secondary infections of the influenza," said Dr. Mark Anderson, an infectious disease specialist at CHI Memorial. "It makes people more likely to have heart attacks, to get bacterial pneumonia, and a lot of other complications, so it led to an increase in hospital admissions."
Erlanger Health System reported almost 1,500 cases of influenza-like illness, or acute respiratory infections, to the health department between Oct. 1 and March 17 this year, compared to about 1,050 during this time last season. The largest number of cases seen in one week was 226 in early February.
Officials at CHI Memorial said the hospital tested nearly 3,900 patients for influenza virus from December to March 19, and more than 660 of those tests came back positive.
Jamie Lawson, a spokesman for Parkridge Medical Center, said the number of new cases dropped significantly over the past weeks, but the infection control department at Parkridge had reported 1,114 flu cases through March 17.
"This year's flu season was unusually severe and challenging to hospitals, not only here but across much of the country," Lawson said, commending providers and employees for their hard work.
Sharon Goforth, special projects supervisor at the Chattanooga- Hamilton County Health Department, said the season's intensity was mainly because flu vaccines are generally less effective against the H3N2 strain of the virus, which was predominant this year.
And while it's impossible to know how many people have been affected by the flu, its impact combined with other seasonal illnesses also caused an increase in health care costs.
Dr. Andrea Willis, chief medical officer at BlueCross BlueShield of Tennessee, the region's largest insurer, said the company has noticed the effects.
In 2017, BlueCross saw a 50 percent increase in the number of inpatient admissions per 1,000 members for influenza compared to 2016. Meanwhile, it saw a 59 percent increase in medical spending.
"Even though the stats and our tracking indicated a bad flu season, the financial impact is limited," Willis said. "For perspective, influenza spending makes up less than .1 percent of our total medical costs annually."
Erlanger CEO Kevin Spiegel said the hospital "saw a tremendous amount of need" as the high volume of sick patients pushed it beyond normal capacity. That will lower revenue, too, since flu patients occupied beds normally used for surgery or other procedures, he said.
"You have to salute the staff," Spiegel said. "It affected us, a lot - it was a little overwhelming."
Many employees also cared for family members or fell ill themselves, including Dr. Larry Shears, chief of cardiothoracic surgery at Erlanger. But Shears also helped save the lives of some of the area's most critically ill.
"The problem is that sometimes it can progress so rapidly," Shears said.
Anderson said respiratory distress and respiratory failure are typically what lead to a critical situation with influenza cases. These individuals are often put on a ventilator, but if they don't improve, extreme measures are necessary.
"We have to go to something called ECMO - that's when we absolutely cannot get oxygen into a person because their lungs are so diseased," he said. "It's obviously a big deal to put someone on that."
Extracorporeal membrane oxygenation, or ECMO, is a temporary support system for patients with severe respiratory or cardiac failure. It restores oxygen to the blood, allowing the heart and lungs to rest, but is used only when conventional therapies are no longer working.
Shears co-directs Erlanger's ECMO program along with Dr. Philip Smith, a surgeon and associate professor at the University of Tennessee College of Medicine at Chattanooga.
When ECMO was first developed, it was used primarily on babies with severe heart conditions, but it has since gained other applications. Smith said doctors started using the machine on influenza patients during the 2009 H1N1, or swine flu, pandemic.
"When H1N1 came along, it was so bad that they were [using ECMO] because they had no other choice, and then they started getting good results," he said.
Smith started the ECMO program at Erlanger in 2013, originally for trauma patients, and estimates the machine was used on one or two flu patients then, but that number has increased every year since.
"It really has revolutionized the way we do influenza in this hospital," he said. "I will tell you the ones that I've put on the pump would not have survived - I can guarantee that."
Between October and March, Erlanger used the technology 28 times, compared to 18 times during the same period a year ago. CHI Memorial, which also has an ECMO program, didn't see an increase in the machine's use this season, but Anderson emphasized its importance.
"If you can get enough oxygen to keep them alive, the ECMO can really be a life-saving thing," he said.
Although viral activity is declining and there is light at the end of the tunnel for providers, flu season may continue for several weeks.
And Goforth said less-effective flu vaccines shouldn't be a reason to forgo the shot. Different strains circulate and the vaccine still affords some protection, even against H3N2. That strain also is notorious for causing higher hospitalization rates.
"If you aren't vaccinated, you have no protection against any of the four strains that we're trying to protect you against," she said.
Still, Anderson said he's worried this season will increase skepticism.
"I think that emphasizes the really great need we have for better vaccine, which researchers are on the verge of making - something that doesn't have to be changed every year," he said. "We really need that, badly."
Contact staff writer Elizabeth Fite at efite@timesfreepress.com or 423-757-6673.