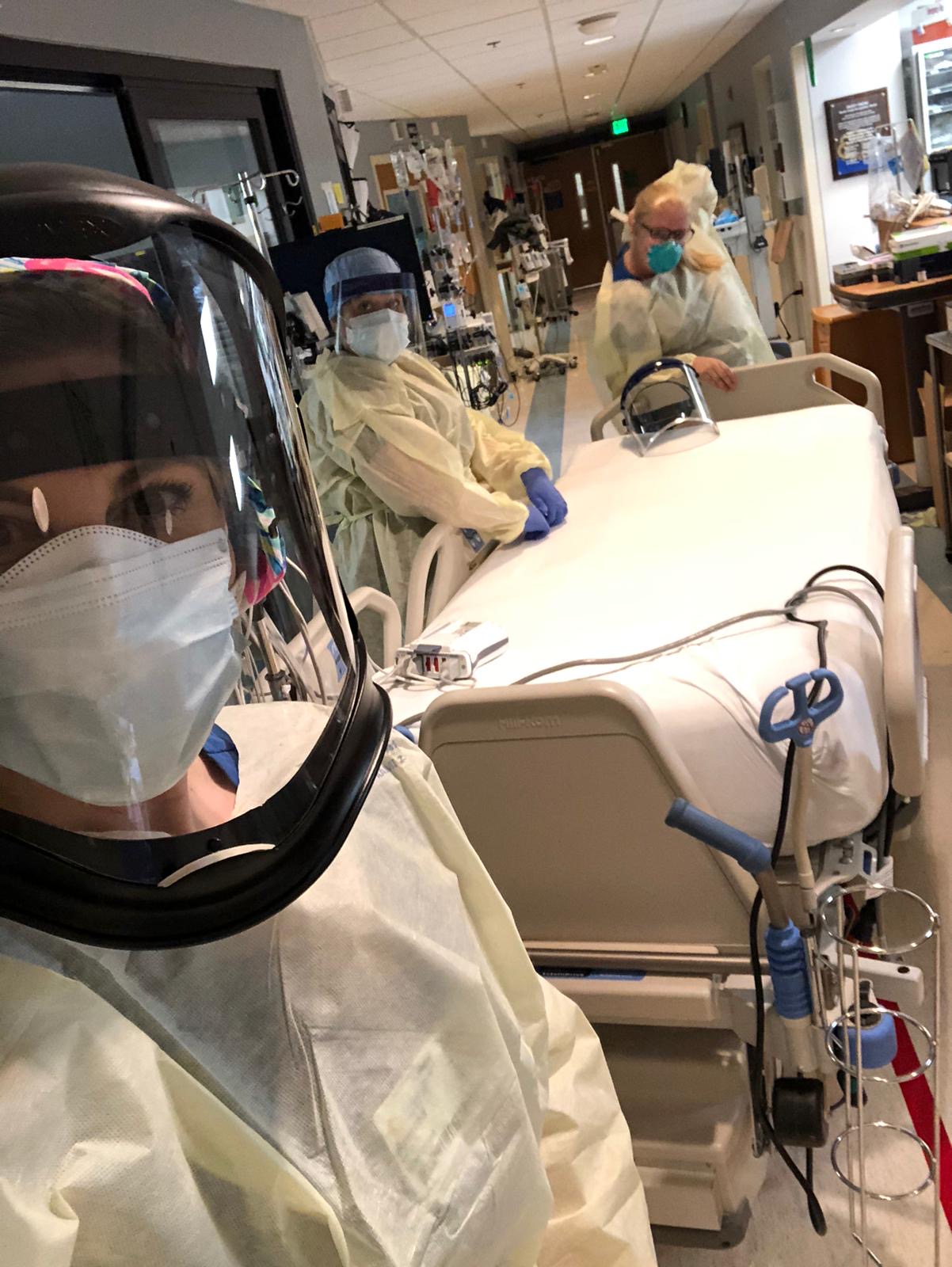
Critical care nurse Victoria Hunter gets home from work around 8 p.m., strips off her scrubs and heads straight to the shower.
She hasn't seen her husband or dog since she left at six that morning but can't risk greeting them with a hug or pet until she's clean. Her husband follows behind to wipe down the doorknob and anything else she's touched.
Although she's physically home, her mind is still on her patients - who are fighting for their lives in the COVID-19 intensive care unit at Erlanger Medical Center.
All day, she's been either at their bedsides or standing in the hall right outside their rooms, watching each breath they take through the window.
She can see their heart rate, blood pressure and oxygen level on computer screens, but monitoring physical changes - if they start to sweat, become delirious or use their abdominal muscles to breathe - requires a trained eye.
If she has to let them out of her sight to perform a task, such as go to the lab, Hunter gives a detailed report of the patient's status to another nurse who keeps watch until she returns.
"They're not just a number for us," she said. "We have emotional connections to these patients. I think about them when I go home. I worry about them."
ICU nurses are used to working in high-stress environments and treating critically ill patients, including those who don't survive, but Hunter said caring for coronavirus patients is different.
Not every COVID-19 patient ends up in intensive care, and those that do may only spend a few days there, but some patients stay in the ICU for months, she said.
"I've never really had as much emotional stress working with patients in the medical ICU," Hunter said. "We definitely have gotten to know our patients really well, because they can't have visitors. We are all they have a lot of times."
Many patients have smartphones or other devices to talk to their loved ones. Although the nurses often help facilitate those conversations, some patients are too sick or cognitively impaired to communicate at all, said Cody Sims, clinical staff leader in Erlanger's medical ICU.
"We just have to be there with them," Sims said. "One of my hardest moments was holding a man's hand as he was passing away and knowing that he couldn't see or contact his family. It really hurt.
"It's really special at the same time that we have an opportunity to be there," he said. "But it's not an alternative to having family."
Tracy Headrick, nurse manager of Erlanger's COVID-19 floor, said one of the biggest misconceptions about the coronavirus is that it only affects older people with chronic conditions.
(READ MORE: Erlanger East nurse tells of her month in New York City fighting COVID-19)
"We have a wide range of patients. I can't pin it down to just one type," Headrick said. "The people who seem to have more problems are the people who have diabetes or respiratory issues, but there's really no rhyme or reason for why somebody is here for a week or somebody is here for a month."
Hunter said nurses are in nearly constant communication with families, relaying messages to patients about their loved ones.
"Whenever families call in, they will usually tell us messages - ask us to tell them that everyone says hi, so-and-so just graduated from high school," she said, but communicating with a patient on a ventilator is difficult.
Typically, patients on ventilators are heavily sedated, so their bodies can relax and allow the machine to take over their breathing.
Even though it seems like they're unconscious and can't hear, Hunter said nurses are taught to always talk to their patients anyway, explaining every procedure, because you never know. Hunter said she stays in the room to keep them company for as long as possible.
"I just hope that they can hear and that they get some encouragement from it," she said.
Aside from the emotional toll, Sims said one of the most difficult aspects of COVID-19 is the effort that goes into personal protective equipment, or PPE.
Before they enter a patient's room, nurses must don their PPE, which includes a face shield, an N95 respirator mask, two pairs of gloves, shoe and hair covers and an impermeable, full-length plastic gown.
In order not to waste PPE, nurses stay in the room between one and three hours, sometimes more if the patient is critical, Sims said.
Once inside, the physical demands can include moving and bathing patients, administering drugs, swapping out equipment, changing tubes and bending down to check wires.
"You pretty much lose a pound of sweat when you're in there," he said.
Hunter said teamwork is key, because nurses can't just go in and out of the rooms.
"That would require taking all their PPE off, throwing it away and putting on new stuff and that's just not realistic," she said, adding that you're more likely to become infected during the process of suiting up or removing PPE.
A COVID-19 patient's condition can change rapidly, so nurses must be mentally and physically on their toes at all times.
Patients on ventilators can't say if their chest doesn't feel right, they're struggling to breathe or they feel nauseated, so nurses rely on their training to try to determine what will happen next. Hunter said it's important to notice small changes before they turn into big ones.
The ever-changing pandemic requires a great deal of flexibility, she said.
"It is kind of astounding the amount of fluctuation there is of how many COVID patients there are in Hamilton County. It doesn't always seem predictable," Hunter said.
Sims said even though there's been a local surge in COVID-19 hospitalizations lately, it's been less stressful than in the early days of the pandemic.
Headrick, the nurse manager, said Erlanger already had a disaster plan in place, but no plan can fully prepare a hospital for a global pandemic of a novel pathogen.
"We started getting prepared for the fact that it might be bad, we might not be able to leave the hospital, we might have to work around the clock," Headrick said.
Even though Erlanger began to prepare early, everyone in the hospital had to be trained in new safety protocols and processes, Sims said.
COVID-19 tests could take days to return, so every patient awaiting results had to be treated as if they were infected.
Now, the hospital has access to rapid testing, and more is known about how to care for COVID-19 patients.
"Everything is a learning curve. At first, we were getting really physically tired, emotionally tired and just drained because it was all new - figuring out how to work in this setting," Sims said. "Now it's like a well-oiled machine - we know exactly what to do, exactly how to do it."
Despite all the challenges, the nurses in the COVID unit have managed to find ways to keep their spirits up.
"I've just been so proud of them," Headrick said. "They don't feel like, 'Why did we have to take the COVID patient?' They're just like, 'Hey, it's time to show up.'"
Hunter said they celebrate the small things, like when a patient who hadn't eaten in days finished a whole serving of mashed potatoes.
"Sometimes our patients are surprised. They're like, 'Why are you so excited about this? Why am I getting all this attention? They don't realize just how invested we are in them getting better," she said.
(READ MORE: Chattanooga nurses go to New York City to help on the front lines of COVID-19 fight)
In the unit, there's a board that shows how many patients have started breathing without ventilators, how many have left the ICU or gone home.
"We're always cheering and happy when we get to change those numbers and add people to it," Hunter said.
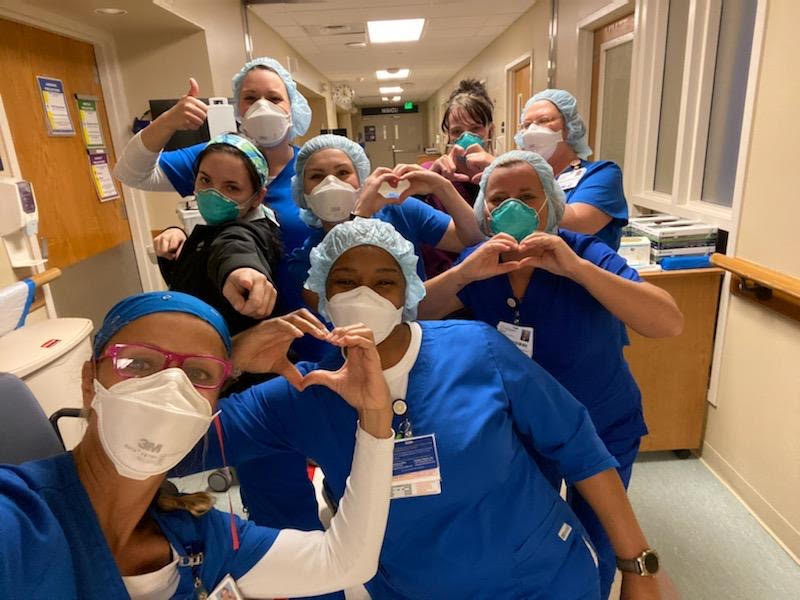 A group of Erlanger nurses who take care of COVID-19 patients pose for a photo on the COVID floor at Erlanger Medical Center. Coronavirus patients are treated on either the COVID floor or in the COVID ICU. Both areas of the hospital are separate from other patients and have negative pressure rooms, meaning potentially contaminated air within the rooms cannot escape. Contributed photo.
A group of Erlanger nurses who take care of COVID-19 patients pose for a photo on the COVID floor at Erlanger Medical Center. Coronavirus patients are treated on either the COVID floor or in the COVID ICU. Both areas of the hospital are separate from other patients and have negative pressure rooms, meaning potentially contaminated air within the rooms cannot escape. Contributed photo.
Sims said the community support is one of the things that keeps him going, whether it's donating food or sending a thank you card.
"The whole thing has just been overwhelming," he said. "It's been tough to get through, and knowing that people care and support you it's something to help you get through the day."
For Headrick, who's worked through mass casualty events and other significant disease outbreaks, the media attention on the coronavirus makes it unlike anything she's experienced.
"It's been several months of being inundated," she said. "People who know that I'm a nurse want to know what I think, and they're thinking the worst. They're thinking that most people who come into the hospital with COVID die, and they think the numbers aren't reported right, and I just try to say, 'No, that's not correct.'"
And although the pandemic shows no sign of slowing down in Hamilton County, Hunter said the hospitals get better at treating COVID-19 patients every day.
She wants people in the community to know that the hospital is safe and ready to treat them should the need arise, and that families' loved ones are in good hands.
"We don't back down, and we do actually care for their loved ones," Hunter said. "I'm also excited when something good happens to them, and we want patients' families to know that - to know that we are completely on their side and are ready to fight this with them."
Contact Elizabeth Fite at efite@timesfreepress.com or 423-757-6673.