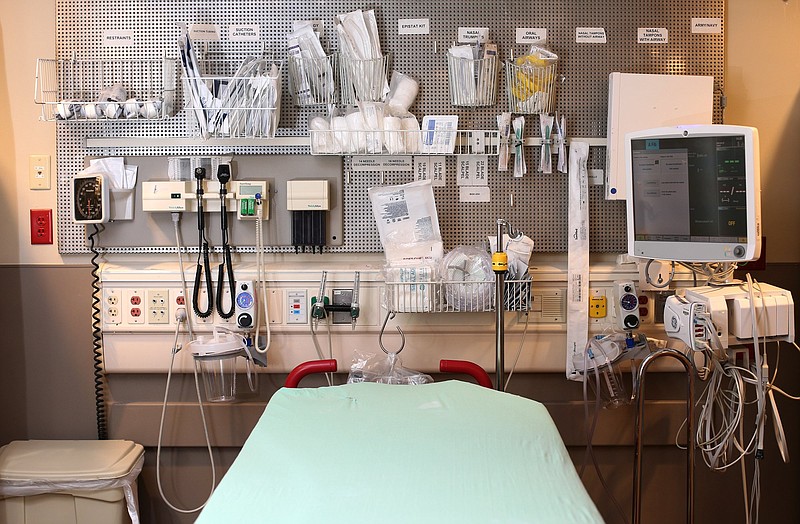
Coronavirus is straining health care systems across the globe, and although Chattanooga has yet to reach its peak number of cases, the pandemic's effect can already be felt in hospitals across the region.
Research and public hospital reports provide a glimpse into how equipped local health systems are to handle a surge in coronavirus patients.
Even with current social distancing measures enacted and sustained, the peak demand for hospital services in the U.S. due to COVID-19 is likely to "exceed capacity substantially," according to an analysis published Thursday by the Institute for Health Metrics and Evaluation at the University of Washington.
The study is the first to generate estimates of predicted health service use and deaths due to COVID-19 by day in each state for the next four months. Researchers found large gaps between the need for hospital services and available capacity, especially for inpatient and intensive care unit, or ICU, beds needed to take care of the sickest patients.
A limited supply of ventilators has also become a chief concern after horror stories emerged from Italian hospitals overwhelmed with coronavirus patients in respiratory failure. Without enough ventilators to go around, doctors were forced to make life-or-death decisions about who would - and who would not - get the machines needed to support their breathing.
Virginia Wolverton, hospital coordinator for the Southeast/Hamilton Regional Healthcare Coalition, fields phone calls and supply requests from local hospitals as part of the area's emergency response. So far, Wolverton said, the primary request from hospitals had been for more PPE, or personal protective equipment - gloves, masks, surgical gowns and face shields.
The coalition has already received two loads of PPE from the Tennessee Emergency Management Agency and distributed those supplies to acute care hospitals across the region. At some point, Wolverton said, they're hoping to receive ventilators, but haven't been told if or when that may happen.
While it's impossible to know for sure when Southeast Tennessee will see its peak number of hospitalizations, the University of Washington analysis projects the state's peak number of cases is coming around mid-April. A separate analysis from Columbia University researchers estimates that with moderate social distancing measures, Tennessee will see the most COVID-19 cases around the middle of June.
Chattanooga Mayor Andy Berke said he tries not to focus too much on projections, since they're unreliable without good data, and a lack of COVID-19 testing means Chattanooga is operating largely in the dark when it comes to knowing how many residents have coronavirus. That's why social distancing measures are so important, he said.
"We want to work hard to keep the spread as slow and as nonexistent as possible so that our hospitals can handle what is coming. We know that the numbers are going to go up. The critical issue is being able to manage them," Berke said.
As of Friday at 2 p.m., 3,823 of 11,481 - or 33% - of hospital beds were available in Tennessee, according to the state's Health Resource Tracking System. In addition, 980 out of 1,460 ventilators, or 67%, were available.
In 2018, Chattanooga had 1,930 total hospital beds, according to the most recent available data from the American Hospital Association and the American Hospital Directory. About 66% of those beds were occupied at the time, which leaves 650 beds open for additional patients, including 250 intensive care unit beds.
An analysis by the nonprofit news outlet ProPublica used mathematical models by Harvard University researchers to estimate the effect on Chattanooga hospitals in a "moderate scenario" in which 40% of the adult population contracts COVID-19 over 12 months. It estimates that about 8% of the adult population will require hospital care - or 1,590 beds over 12 months - which is 2.4 times more than what's normally available.
The analysis also found that intensive care units in the area would be especially overwhelmed. Without coronavirus patients, on average there are only 59 available beds in intensive care units - 5.9 times less than what is needed to care for the projected amount of severe coronavirus cases.
Most people with COVID-19 have mild illness and are able to recover at home without medical care. For patients with COVID-19 who require hospitalization, some experience mild illness for a few days and develop more severe illness about a week later. Others progress to severe disease quickly. About 80% of deaths and 45% of hospitalizations for COVID-19 in the U.S. are among adults aged 65 or older, with the risk of serious illness and death increasing with age, according to the U.S. Centers for Disease Control and Prevention.
Local hospitals repeatedly declined to answer questions about their COVID-19 preparations, including whether they had increased their bed capacity, how many patients were now in the hospitals and if they had closed floors to prepare for a COVID-19 patient surge.
Last week, CHI Memorial, Erlanger and Parkridge Health Systems announced they would suspend elective surgeries to preserve vital health resources and save room for an influx of patients. But exactly how many supplies are currently on hand and when local hospitals expect to see a surge in COVID-19 cases - or already have - remains unclear.
In a joint statement sent late Friday afternoon, CHI Memorial, Erlanger and Parkridge spokespeople said, "Our medical and emergency response teams are working tirelessly to meet the demands and communication needs related to emergency preparedness, facility operations and patient care. Please know we are not avoiding your questions. We have been working even harder than usual to get the answers. We are just exceptionally challenged these days to meet your deadlines given our communications roles in the organization."
Some hospitals have chosen to be more open about how they're handling coronavirus.
Hamilton Medical Center in Dalton, Georgia, publicly announced confirmed cases at the hospital and posts test results on its website. So far, four patients have tested positive for the virus.
Jeff Myers, president and CEO for Hamilton, said in an email that the health system wants to be "as transparent as possible" in order to educate the community.
"We also want people to take it seriously - not panic - but truly take every precaution to keep everyone as safe as possible," Myers said.
Dr. Paul Biddinger, chief of emergency preparedness at Massachusetts General Hospital, said during a webcast this week that hospital capacity is always a challenge during disasters. Like other hospitals, Massachusetts General has pared down to essential services, which Biddinger said has hovered around 60% capacity for the week when it's normally more than 90% full.
"That's both a good and a bad number - 60% is a lot better than 90% in terms of what we expect we are about to see," Biddinger said. However, it also means that the hospital is still two-thirds full with people who need medical care, including childbirth, stroke, heart attacks and trauma.
"We are absolutely anticipating a large wave of patients as we've seen elsewhere in the world," Biddinger said. "When you ask me what I'm most concerned about, it's what's still coming."
Contact Elizabeth Fite at efite@timesfreepress.com or 423-757-6673.