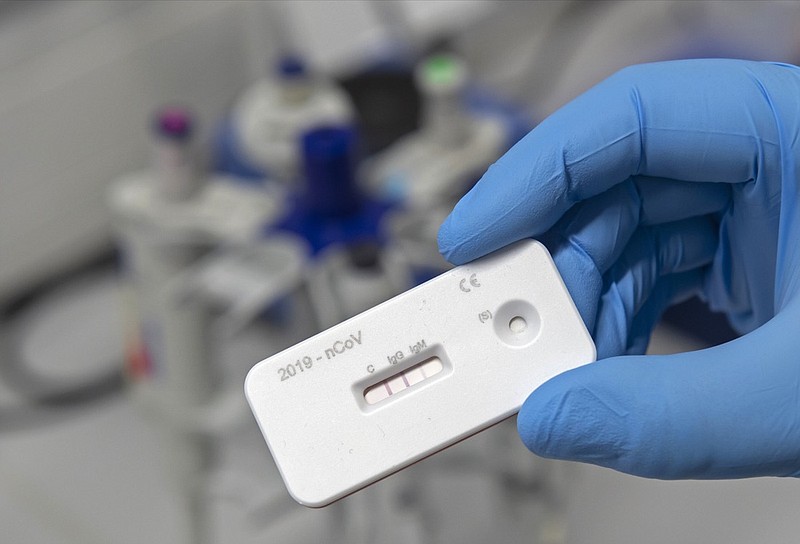
As area businesses begin to reopen and residents are venturing out in public, federal regulators are warning states and consumers about the potential for fraudulent COVID-19 antibody tests.
When accurate, antibody tests - a type of serological or blood test - can show whether a person or population was exposed to COVID-19. That's because those who have recovered from COVID-19 will likely have antibodies to the coronavirus in their blood.
Scientists and public health leaders say these tests could help control the pandemic by providing important information on disease prevalence and the frequency of asymptomatic infection. But with more than 100 COVID-19 antibody tests currently on the market - only a handful of which have received emergency authorization from the U.S. Food and Drug Administration - and a push to use them as part of America's reopening strategy, the FDA issued new guidance and a warning on Monday:
"We unfortunately see unscrupulous actors marketing fraudulent test kits and using the pandemic as an opportunity to take advantage of Americans' anxiety," reads an online statement from FDA officials. "Some test developers have falsely claimed their serological tests are FDA approved or authorized. Others have falsely claimed that their tests can diagnose COVID-19 or that they are for at-home testing, which would fall outside of the policies outlined in our March 16 guidance, as well as the updated guidance.
"Also, since that time, the FDA has become aware that a concerning number of commercial serology tests are being promoted inappropriately, including for diagnostic use, or are performing poorly based on an independent evaluation by the NIH," according to the statement. "We encourage states, hospitals and consumers to be on high alert and to make informed purchasing decisions regarding these tests."
Only 12 antibody tests have currently received emergency use authorization, most within just the past few days, according to the FDA website. This authorization is reserved for emergency situations and requires less vetting to obtain than full FDA approval.
The warning came after a group of research scientists compared a dozen COVID-19 antibody tests and found that many of the test kits have false positive rates that could indicate a large proportion of those testing positive may not actually have had COVID-19.
"It's the Wild West right now. These tests are widely available, and many people are buying and deploying them, but I realized that they had not been systematically validated, and we needed to figure out which ones would really work," Patrick Hsu, an assistant professor of bioengineering at UC Berkeley leading the effort, said in a news release. "This is a huge, unmet need for public health."
Some government officials and lawmakers have pushed for more access to COVID-19 antibody tests, saying they will help save lives and restart the economy sooner by determining who is - at least temporarily - immune to the disease. However, more information is needed on how the immune response to COVID-19 works before assuming that antibody tests can safely predict protection from future infections, the researchers cautioned in the news release.
Alyssa Summers, a molecular biologist and professor at the University of the South, is currently working to test local samples for COVID-19 at the Baylor School lab.
Summers said there are currently two main types of antibody tests on the market. One requires a more sophisticated lab technique, and the majority that are being used and reported on are called "lateral flow" tests.
Lateral flow tests use a finger prick to detect antibodies from whole blood at the point of care. The tests behave similar to pregnancy tests, but instead of urine, a provider places a drop of blood on a strip of paper allowing the blood to flow across.
The tests that use whole blood and are run on the lateral flow systems have been less likely to correctly identify those with the disease (true positive) and those without the disease (true negative) and often "cross react" - meaning they detect antibodies for another disease - with some influenza viruses or other coronaviruses, Summers said.
The other type (serum and plasma testing) requires an intravenous blood draw. The sample is then run through a high throughput system to test for antibodies. Baylor is currently exploring one of those systems, which Summers said shows higher specificity and sensitivity for just SARS-CoV2.
"They've tested against these other coronaviruses as well as other influenzas and they don't cross react," she said. "But they [all antibody tests] are not all made the same, so I think that's where you're seeing some of the confusion."
No test is 100% accurate, and Summers said just because something is uncertain doesn't mean it's necessarily not worth testing and using responsibly.
"Even with a vaccine, you're not necessarily 100% immune for life, for example adults often need boosters to some of their early childhood vaccinations," Summers said. "A lot more studies have to be done to understand how much immunity you get [from the coronavirus].
"The immune system is complex."
Contact Elizabeth Fite at efite@ timesfreepress.com.