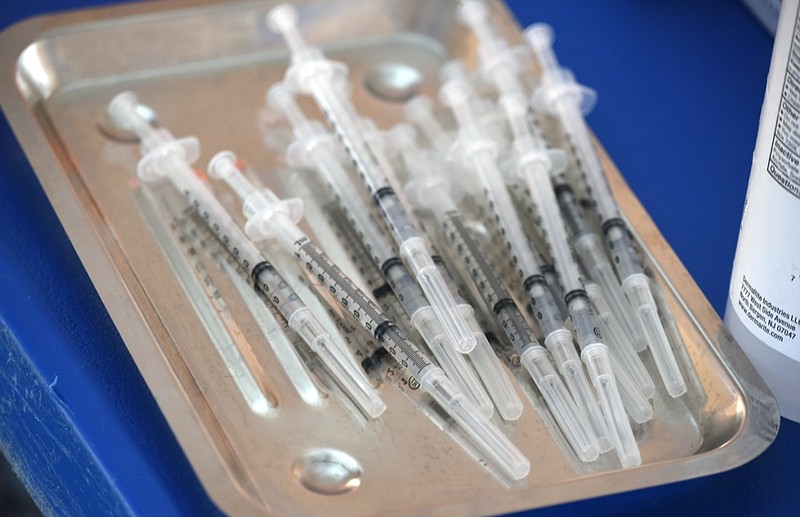
Note: This is the fifth in a series of stories about the concerns of people who are hesitant to receive the COVID-19 vaccination. Read previous installments at timesfreepress.com/covid.
Front-line health care workers were the first in line when COVID-19 shots became available in December, but polling shows that medical professionals can be vaccine-hesitant, too, leaving some with concerns about the vaccines to question whether health care professionals know something the rest of us don't.
As of early March, 52% of front-line health care workers reported having received at least one dose of a COVID-19 vaccine and 42% said they had received both doses - meaning half of front-line health care staff remained unvaccinated at the time, according to a survey of front-line health care workers conducted by The Washington Post and Kaiser Family Foundation in April.
A separate survey of 160 rural hospital leaders conducted by the Chartis Center for Rural Health between March 12 and April 15 found that nearly half of respondents reported that between 21% and 50% of their staff had decided not to get a COVID-19 vaccine.
"When asked why health care personnel are declining a COVID vaccine, a majority of respondents - 44% - cited 'Matter of Personal Choice,'" according to the survey, which was reported in the industry publication Fierce Healthcare.
"Another 31% reported a lack of trust in vaccines," according to the article in Fierce Healthcare.
This week, the Times Free Press has been tackling some of the common questions surrounding COVID-19 vaccine safety starting with, "How can the COVID-19 vaccines be safe if development was rushed?"; "What's in a COVID-19 vaccine?"; "How do the COVID-19 vaccines work?"; and "How common are adverse events, and how do we know there won't be long-term effects from COVID-19 vaccines?"
With this final installment, we'll look into:
Question: If COVID-19 vaccines are so great, why don't more health care workers take them?
Answer: Health care workers can experience the same drivers of vaccine hesitancy as the general population, and many of the vaccination trends among medical staff mirror disparities found in vaccination rates across the country.
The type of setting where medical staff go to work, their education, political beliefs, religious beliefs, where they live and their race and ethnicity can all factor into their decision to get vaccinated.
An ongoing research project from the Kaiser Family Foundation tracks the evolving public attitudes toward COVID-19 vaccinations. According to the foundation's research, unvaccinated adults are usually younger, people of color, Republican-leaning and less-educated.
"But unvaccinated isn't an entirely uniform group, with significant differences by intention," the report states. "Adults who want to 'wait and see' before getting vaccinated are more likely to be young and people of color, while those in the 'definitely not' group are more significantly Republican-leaning and in rural areas."
Dr. Matthew Kodsi, vice president of medical affairs at CHI Memorial Hospital, said that like all people, health care workers are not immune from what's happening in the community at large.
"We've [CHI Memorial] done a lot of the community vaccination events, and we've seen our numbers go down from when we did 2,000 in one day back in March, and now if we can do 20 at a time we're jumping up and down with excitement," Kodsi said. "So it's just everyone has these concerns that are unfortunately, in many cases, due to misinformation."
One of the biggest concerns he said he's heard among women - which comprise 76% of the health care workforce, according to the U.S. Census - is the fear that vaccines will cause infertility, "which has no scientific foundation."
"People might say, 'Well, you don't know. We haven't followed it for 10 years,'" he said. "True, I'm not going to say that we have long data. But what we have is science that says there is no medical reason to expect that that would happen. And there is data looking at people who are pregnant - tens of thousands of people who are pregnant who've been vaccinated, or more - and it shows no increased risk of miscarriage. So, there's no reason to believe that that's a risk."
Dr. Rupali Limaye, who is an associate scientist at Johns Hopkins Bloomberg School of Public Health, said that vaccine hesitancy in the African American community is "not only due to historical perception of medical experimentation but also current racism and discrimination. And then there's also issues related to the vaccine product itself. Is the vaccine safe for Black people? Is it safe for individuals that might have diabetes, et cetera?"
In the poll by The Washington Post and Kaiser Family Foundation, 39% of Black front-line health care workers and 44% of Hispanic front-line health care workers reported receiving a COVID-19 vaccine as of early March, compared to 57% of white health care workers.
In the general population and in health care, education is one of the strongest predictors of vaccine acceptance.
Workers involved in diagnosing and treating patients, such as doctors and nurses, were the most likely to be vaccinated, according to the poll, with 68% reporting having received at least one shot compared to those who assist with patient care, such as bathing, eating, cleaning, exercising and housekeeping. In the pool, 37% of people who assisted in care were vaccinated.
Staff working in hospitals and outpatient clinics reported the highest rates of vaccination as of early March, with 66% and 64%, respectively, saying they'd received a shot. But rates were lower among doctors' office staff (52%) and nursing homes or assisted care facilities (50%).
One in four (26%) home health care workers - a job that requires no formal educational credential and pays around $10-$12 per hour - reported getting a vaccine.
Kodsi said that the hospital is continuing to educate both staff and the public about vaccine safety, and often the best tool to overcome hesitancy is an individual conversation with a person. He recalled talking to a group of people at a recent vaccine event who were debating whether or not to get vaccinated.
"We had a really good conversation. It took us about 10 or 15 minutes, and they then felt comfortable getting the vaccine and did," Kodsi said. "The most important thing we as a system and a community and health care workers can do is to make sure that everyone who makes the decision about whether or not to receive the vaccine is making that decision with as much accurate information.
"We don't want people to feel like we're just going to tell them they've got to get it," he said. "We want to respect their concerns, address their concerns, make sure they've got the information they need so that they can make the decision that really is the best for them."
Contact Elizabeth Fite at efite@timesfreepress.com or follow her on Twitter @ecfite.