A device that retrieves blood clots from the brain after a stroke, radiation delivered immediately after surgery for breast cancer and the latest leukemia treatment for children -- those are just a few of the devices and clinical trials undergoing testing in Chattanooga area hospitals.
Once primarily done only in large teaching hospitals, in the last several decades research has shifted and doctors and clinicians now conduct clinical trials in most hospitals across the United States.
On its website, which tracks clinical trials around the world, the National Institutes of Health list more than 6,000 trials in Tennessee, with about 700 of those in Chattanooga. Of the three local hospitals, Erlanger Health System conducts the most trials, with more than 200 ongoing, but officials at Memorial Health Care System and Parkridge Medical Center said their hospitals also are engaged in clinical trials.
"I think we've seen the community of physicians becoming increasingly engaged in clinical research," said Dr. Colleen Schmitt, the medical director who heads up research at Memorial. "It brings value to our community and value to our patient population."
At Memorial, doctors are conducting a wide variety of trials, including research on heart disease and cancer, Schmitt said. The hospital has about 20 ongoing trials, she said.
Chattanooga doctors involved in research said clinical trials allow them to offer safe and tested technology to patients who could not receive it otherwise and also to provide the treatment at no cost to the patients.
The majority of trials are done for drug companies or device makers, but some are also "homegrown," with doctors initiating their own research. Whatever the type of trial, they are monitored by the National Institutes of Health.
The trial process is rigorous, the doctors said, and must first undergo several testing phases before it can be conducted on patients. In addition, any trials must be approved by institutional review boards and research programs to ensure the hospitals have the proper resources to conduct a specific trial.
The process takes an enormous time commitment, from filling out the required paperwork to tracking patients and documenting all the results, but doctors said they jump through the hoops because trials provide patients access to cutting-edge treatment.
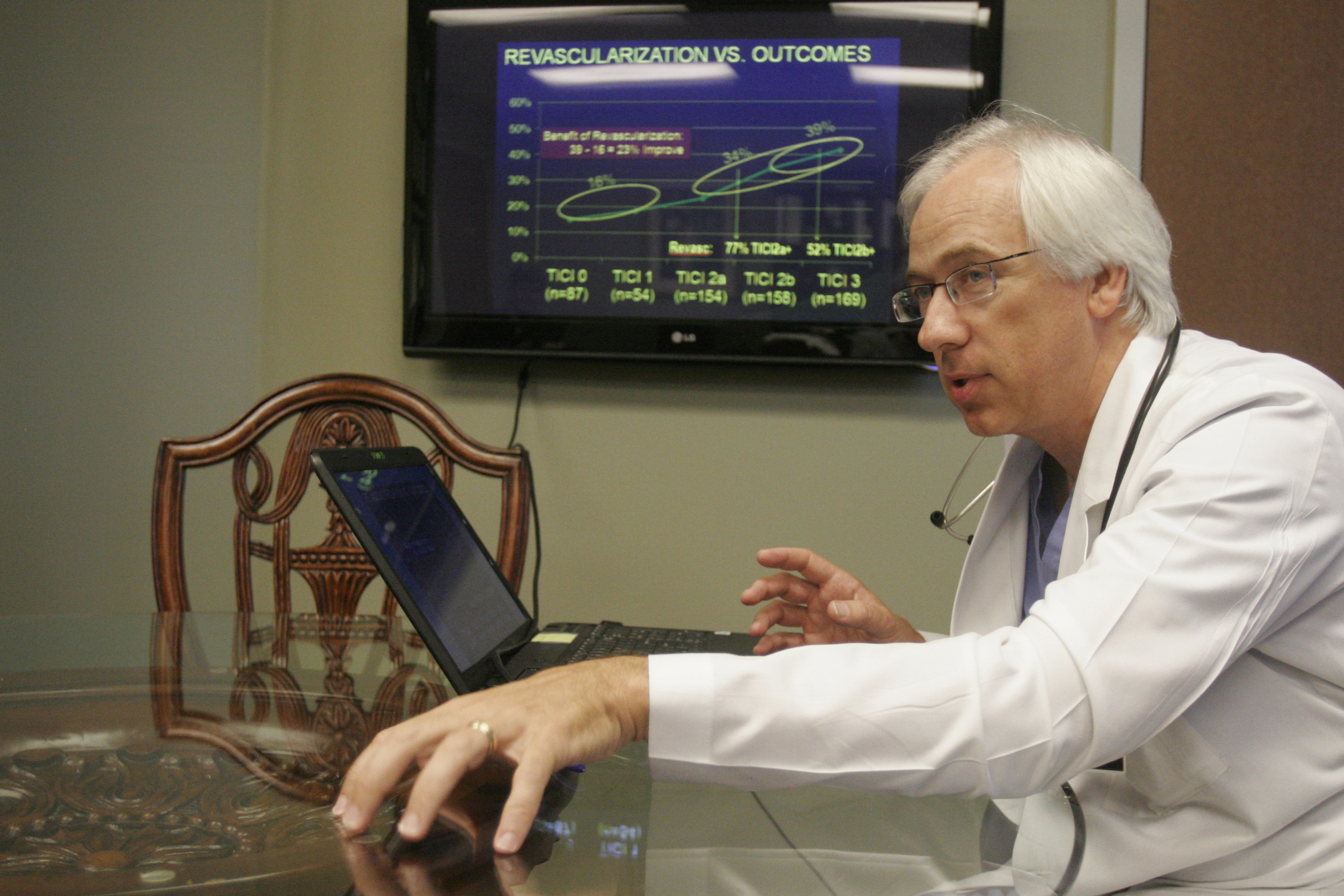
"It gives patients hope," said Dr. Tom Devlin, director at Erlanger's Southeast Regional Stroke Center. "It is a very different statement to say, 'That is all that can be done,' rather than, 'That is all we can do.'"
Devlin and his team, including Dr. Blaise Baxter, test treatments and devices on stroke patients. Trial devices being tested or on the cusp of testing include devices to retrieve blood clots in the brain after a patient has a stroke, medication to dissolve clots and an Israeli device that stimulates the brain to help restore blood flow after a stroke.
Chattanooga serves as a hub to treat stroke patients for a large regional area that is sometimes known as the "stroke capital" of the country. Because brain cells die quickly after a stroke and the sooner a patient can get treatment, the better the chances of recovery, having access to such treatments can mean a difference to a large number of patients, Devlin said.
During a recent interview at his office, Devlin showed videos of patients receiving the trial treatments who recovered more rapidly and completely than they would have with conventional treatments. Devlin's enthusiasm for his work was evident as he described each treatment, talking for two hours about the importance of the new treatments and how they can change the lives of patients.
At Parkridge, an ongoing clinical trial of another device -- the TruePath -- also clears blocked arteries but in peripheral arteries, especially in the arms or legs. Parkridge has 17 ongoing trials, with 13 led by physicians and four by the hospital.
Dr. Christopher Lesar, a vascular surgeon, calls the research he does in clinical trials "professionally satisfying" for such devices as the TruePath.
"The problems we deal with are horrible problems -- limb-threatening and life-threatening," Lesar said. "We are helping people and helping make the device better."
In another wing at Erlanger, Dr. Manoo Bhatka works with a different type of clinical trial -- cancer treatment for children. In his decades of cancer research and treatment, Bhatka has seen survival rates for children diagnosed with cancer rise from 30 percent in the 1970s to about 95 percent today. Some rates are as high as 98 percent, largely because of constant research, innovation and pushing for the latest treatments, he said.
"It's an exciting world to me," said Bhatka, who described being able to tell parents their children can get the latest available treatment.
Patients should remember that clinical trials have been tested extensively before they are tested on patients, Bhatka said, which means the treatment is safe. Many cancer treatment trials for children now focus on reducing the amount of medicine and treatment while still providing the same results, he said.
Five-year-old Seth Carpenter is a patient in one such trial. His mother, Robin Carpenter, said they never hesitated about enrolling Seth in the trial when he was diagnosed with leukemia 19 months ago.
"We knew it was as good, if not better, than the treatment he would have gotten otherwise," she said.
Over the last few decades, the shift in clinical trials from government-sponsored and led by teaching hospitals to wider options of how trials are conducted makes the field more vibrant and rapidly evolving, doctors say.
Private companies provide the innovation and funding, while government agencies carefully monitor and scrutinize the safety and effectiveness of the research, Devlin said.
"It's a very good balance," Devlin said. "It's not perfect, but the series of checks and balances works very well."
Contact staff writer Mariann Martin at mmartin@timesfreepress.com or 423-757-6324.