There is good, bad and ugly - and perhaps we should add missing - news on COVID-19 early in this week No. 10 of Southeast Tennessee's coronavirus chronicle.
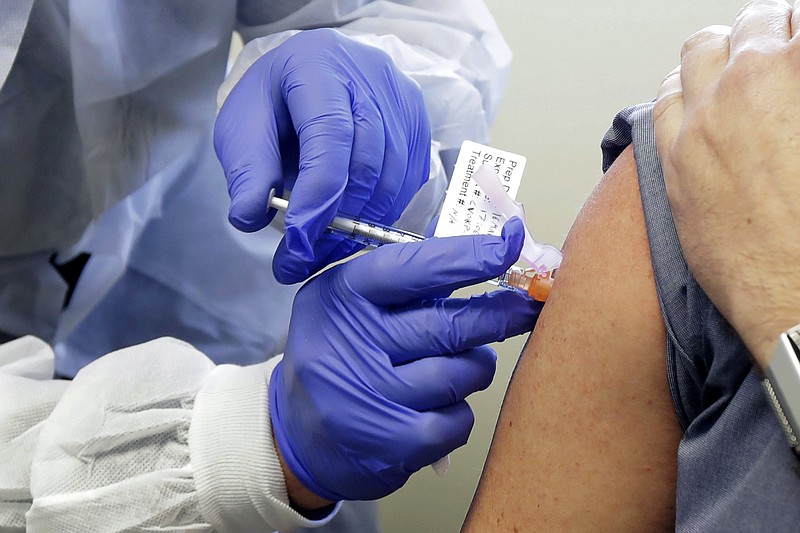
The good news is that an experimental vaccine - one of eight in the works worldwide - is showing promising early signs that it can create an immune response in the body that could help fend off the novel coronavirus, according to sampling of data from a small, first human trial of inoculation.
In 25 people who received a test shot, researchers reported that their levels of antibodies equaled or exceeded the levels of antibodies found in patients who had recovered from the virus. In eight, the vaccine successfully stimulated the body to create antibodies capable of neutralizing the virus in a test tube, meaning the virus could no longer infect cells. That second number may rise, officials said, as that particular test takes longer to perform.
A phase two trial is expected to begin shortly, and the final-stage trial could begin in July, according to officials with the drug company Moderna Inc., which is running the trial with the U.S. government and a grant of up to $483 million. With this news, Moderna shares surged 26% in trading, according to Bloomberg News.
Secondary good news is that Tennessee is one of 10 states to reach a benchmark for COVID-19 testing. The benchmark, set by Harvard researchers, called for the state to perform 3,266 tests daily by May 15 to track and contain the virus. Tennessee in the past seven days averaged 9,059 tests a day.
Georgia and Alabama did not meet their higher benchmarks, which were based on their outbreaks and populations. Georgia needed 25,979 tests a day but averaged 9,059. Alabama needed 8,817, but tallied 4,133 a day.
Knowing who's infected, isolating those people and identifying people they've contacted so those folks can be tested are key to containing the virus while we await a vaccine. And a vaccine will be crucial to really lift our economy.
Now for the bad news. Meeting our testing benchmark is by no means a fix. In fact, meeting the benchmark means testing only "at least 2% of our population monthly." State officials will make decisions about reopening - or re-closing - based only on meeting that goal.
As for the missing news, we're talking about the people who are missing in the testing and treatment processes.
We know, thanks to a Nashville-based analytics company, that Hamilton County is especially vulnerable to COVID-19 because of its demographic and other factors - like high numbers of minorities and people living in poverty. We also know, based on contact tracing, that beginning last week, areas of the city's south side began surging in confirmed cases, especially from the ZIP code 37407 which includes East Lake and Clifton Hills. One of every six confirmed local cases is coming from that high minority, low-income community.
Yet the Hamilton County Health Department does not collect data on the race or ZIP code of those being tested, making it unclear which segments of society are being reached by its push to increase testing. While we cannot say testers are deliberately leaving out minorities and poor people, we can absolutely say they have had, until very recently, no real plan to seek them out.
This week, the Unity Group in Chattanooga called on the health department to develop such plans. There is no excuse for not doing this. It's just one more question and box to check at the testing station. Unless, shame on us, we just don't want to know.
Finally, for the ugly news: At the very time we most need our highest government officials to model good disease management, our president not only dismisses face coverings and social distancing, he turns to a medication roundly panned as unsafe and ineffective.
President Trump on Monday told reporters he is taking a malaria drug, hydroxychloroquine, to protect himself against COVID-19 despite his own government's warning that the drug should only be administered in a hospital or research setting because of potentially fatal side effects. Trump, who has pushed the use of this drug, says he's been taking it "for about a week and a half now." He said he requested it from the White House physician.
Recalling Moderna's shares surge makes us wonder if Trump's embrace of hydroxychloroquine has any financial meaning to him, his family or some favored donors.
Drug and vaccine research hasn't always been built on money. Jonas Salk, who developed the polio vaccine in the early 1950s, tested it first on his own healthy children and never filed a patent.
"He refused a patent for his work, saying the vaccine belonged to the people and that to patent it would be like 'patenting the Sun,' according to a Discover Magazine article written in April by Carl Kurlander, a senior lecturer at the University of Pittsburgh where Salk conducted his research, largely funded by the public through the March of Dimes.
When it was time to roll out 400 million vaccines between 1955 and 1962, doctors bought them for $1.50 a dose and sold them to their patients for $5. By the end of the century, polio was a memory.
So much for market shares.