In 2019, following a late-night steak dinner, Dawn Ford's husband, Robert, woke up covered in hives.
"He tends to have allergies, like to wasp stings, so I wasn't initially alarmed," Ford says of her husband's reaction that night. He took Benadryl, went back to sleep and woke up fine, she says.
But then it happened a second time — again following a steak dinner.
Perplexed, Robert began researching his symptoms, which is how he learned about alpha-gal syndrome, a condition that causes an allergy to red meat and other mammal products and usually begins with a tick bite.
Ticks: the bane of summer fun. They're creepy, crawly and can transmit a host of diseases, now including alpha-gal syndrome, first discovered in 2009.
(READ MORE: How to prevent tick and mosquito bites as the weather heats up in the Chattanooga area)
According to the U.S. Centers for Disease Control and Prevention, reported cases of tick-borne diseases, such as Lyme and Rocky Mountain spotted fever, doubled between 2004 and 2016.
Ford, an epidemiologist and professor of public health at the University of Tennessee at Chattanooga, says that increase is partly due to climate change. Ticks go dormant in cold weather, but shifting seasons allow them to remain active more days of the year, she explains.
Moreover, a 2016 assessment of climate and health, federally supported by the U.S. Global Change Research Program, found that these warming trends not only allow ticks to have a longer season but also to expand their range northward.
But Ford says, "We don't need to be scared of ticks. We just need to be aware of them. Animals transmit diseases all the time. Bats transmit rabies; birds transmit bird flu. We tend to just be more easily exposed to ticks, especially in Chattanooga, where we tend to be outside a lot."
Here's what to know about protecting yourself against ticks this summer.
There are six species of tick found in Tennessee, but only three pose a real threat to humans, Ford says. Those include the American dog tick, the blacklegged tick and the lone star tick.
 Getty Images / American dog tick
Getty Images / American dog tick
American Dog Tick
How to ID: Among the three tick species to know about in East Tennessee, the American dog tick is the largest, about 1/4-inch long, or the size of the width of a pencil. The female is reddish-brown with a creamy-white "shield" marking on its back, directly behind the head. The male is also reddish-brown but with creamy-gray markings covering the back, giving it a mottled appearance.
Associated illness: Rocky Mountain spotted fever.
This bacterial disease is spread through the bite of an infected dog tick. It is the most reported tick-borne disease in Tennessee, according to the Tennessee Department of Health, with 88 cases reported in 2022.
Symptoms and treatment: Early signs include a headache, fever and rash, with the spotted-fever rash appearing as red splotches or pinpoint dots. Other signs may include nausea, stomach pain and muscle pain. Symptoms may take a week or more to develop. If caught early, spotted fever is easily treated with antibiotics.
Good to know: The brown dog tick is a similar species also found in East Tennessee that can transmit Rocky Mountain spotted fever. It is reddish-brown and about half the size of the American dog tick. However, it rarely bites humans, preferring to live on dogs or other small mammals such as rabbits.
 Getty Images / Blacklegged or deer tick
Getty Images / Blacklegged or deer tick
Blacklegged or Deer Tick
How to ID: The blacklegged tick, also known as the deer tick, is the smallest tick of the three species to know about in the region. It is less than 1/8-inch long, or the size of the width of three stacked pennies. It is reddish brown with a black spot behind its head.
Associated illness: Lyme disease.
Caused by the bacteria Borrelia burgdorferi, this is the third most common tick-borne disease in Tennessee. According to the Tennessee Department of Health, the state saw 30 cases in 2022.
Symptoms and treatment: Symptoms commonly include fever, headache, swollen lymph nodes and a rash resembling a bull's-eye. The hallmark rash occurs in 70-80% of those infected and may take anywhere between three to 30 days to develop, according to the Centers for Disease Control and Prevention. Caught early, Lyme disease can be treated with antibiotics.
Good to know: Lyme disease is the most common vector-borne disease in the U.S. The Centers for Disease Control and Prevention report that approximately 476,000 Americans are treated for Lyme disease each year. The majority of these cases occur in Northeastern states.
Lone Star Tick
How to ID: Larger than the deer tick but smaller than the American dog tick, the female lone star tick is easily identified by the trademark white dot on its back. The males have spots or streaks of white pigment around the edge of their bodies.
Associated illness: Alpha-gal syndrome.
Also called red-meat allergy, this condition was first discovered in 2009. That year, 24 cases were reported. By 2020, 34,000 cases had been identified nationwide, according to a study published by the National Institutes of Health.
The Centers for Disease Control and Prevention reports that the states with the highest number of people testing positive for the allergy are Arkansas, Virginia, Kentucky, Oklahoma and Missouri.
Symptoms and treatment: Symptoms of alpha-gal syndrome include hives, itchy rash, nausea, heartburn, diarrhea and swelling of the lips, throat, tongue or eyelids, usually occurring 2-6 hours after eating meat or dairy. Reactions can range from mild to life-threatening. According to the Mayo Clinic, there is no treatment other than avoiding red meat and other alpha-gal-containing products. However, studies show that the condition may lessen or even disappear over time, especially in those who avoid additional tick bites.
How it works: Alpha-gal is a sugar molecule, or carbohydrate, found in the meat of most mammals (pork, beef, rabbit, venison, etc.). It is also found in products made from those animals, such as gelatin and milk. Trace amounts of alpha-gal can turn up in some medications and household items, such as deodorant and laundry detergent, via byproducts — which may also cause a reaction.
"It's a life-changing disease," says Ford, who describes her husband as a "meat-and-potatoes guy."
"It was very distressing for him to have to avoid red meat and carry around an EpiPen just in case."
For some, the syndrome may be lifelong, but luckily for Ford's husband, Robert, his symptoms did eventually disappear, and he can now, again, enjoy a steak dinner.
 Getty Images / The size of a fully engorged female deer tick can approach the size of a raisin.
Getty Images / The size of a fully engorged female deer tick can approach the size of a raisin.
Tick-borne diseases you've probably never heard of (but that are on the rise in Tennessee)
The Centers for Disease Control and Prevention calls ehrlichiosis (pronounced "err-lick-ee-oh-sis") and anaplasmosis, "two tickborne diseases that might not be on your radar, but that should be."
The illnesses are similar, causing flu-like symptoms such as fever, muscle aches and headache, usually appearing within 14 days of a tick bite.
The Mayo Clinic reports, "If treated quickly with appropriate antibiotics, you'll likely recover within a few days."
However, if left untreated or misdiagnosed, they can lead to serious or life-threatening complications.
Here's what else you should know.
Ehrlichiosis
In 2017, the CDC reported in its Emerging Infectious Diseases journal that ehrlichiosis was "grossly underreported," likely due to a lack of awareness about the disease.
In Tennessee, ehrlichiosis is caused by lone star and blacklegged ticks.
In 2022, Tennessee reported 73 cases, making it the second most reported tick-borne disease in the state. What's more — according to the Tennessee Department of Health, a startling 64% of those cases required hospitalization.
Anaplasmosis
In Tennessee, anaplasmosis is caused by the blacklegged or deer tick, a species that is currently expanding its range in the Tennessee Valley, according to a 2018 study published by the National Institutes of Health.
The state department of health reports a "significant increase" in cases of anaplasmosis between 2021 and 2022, jumping from 10 to 13 reported cases.
"It's important to note that most tick bites will not result in disease," Ford says.
So when should you see a doctor?
If you are bitten by a tick, Ford recommends monitoring for symptoms, which may take a week or more to develop. Symptoms are similar for all the tick-borne diseases found in Tennessee, which commonly include headache, fever and rash.
If you experience any of those following a tick bite, call your health care provider.
"By and large, [tick-borne diseases] are treatable," says Ford, adding "We are far more likely to get a foodborne illness like salmonellosis or camphylobacteriosis than a tick-borne disease."
 Getty Images / Pets can get tick-borne illnesses, too.
Getty Images / Pets can get tick-borne illnesses, too.
Can pets get tick-borne illnesses, too?
Yes. Just like humans, dogs and cats can contract Rocky Mountain spotted fever, Lyme disease, ehrlichiosis and anaplasmosis from infected ticks.
If your pet is bitten, you should monitor for symptoms which may include rash, fever, lethargy, bruising, poor appetite, nose bleeds and/or joint swelling or pain — usually occurring 1-3 weeks following the bite of an infected tick.
The verdict is still out on whether or not pets can develop alpha-gal syndrome, the red-meat allergy. Until recently, it was generally accepted that they could not.
Here's why: Alpha-gal is a carbohydrate present in all mammals except apes and humans. Because dogs and cats already have the alpha-gal carbohydrate in their bodies, it seemed unlikely they would create antibodies to attack it, which is what causes the reaction.
But a 2019 National Institutes of Health study found evidence that dogs could possibly develop an allergy to meat similar to that in humans via a tick bite. Research is ongoing.
The best defense for your pets is always to talk to your veterinarian about tick prevention products.
Debunking myths about ticks
> NOT all ticks carry disease.
> All ticks DO bite, regardless of sex or age. (Yes, even larvae can transmit disease if infected.)
> Applying petroleum jelly or dish soap to an attached tick will NOT encourage it to withdraw from the skin.
> Applying a flame or hot matchhead to an attached tick will also NOT encourage it to withdraw.
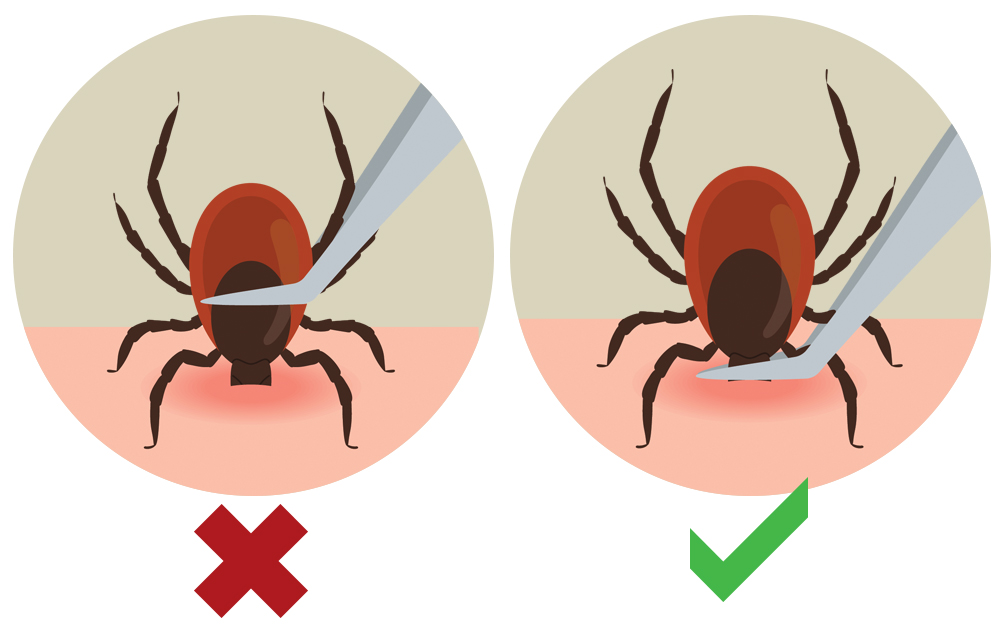 Getty Images / Illustration by Matt McClane / To remove a latched tick, use clean, fine-tipped tweezers and grasp the tick as close to the skin's surface as possible. Pull up with steady, even pressure and do not twist or jerk the tick.
Getty Images / Illustration by Matt McClane / To remove a latched tick, use clean, fine-tipped tweezers and grasp the tick as close to the skin's surface as possible. Pull up with steady, even pressure and do not twist or jerk the tick.
How to remove a tick
1. Use clean, fine-tipped tweezers.
2. Grasp the tick as close to the skin's surface as possible.
3. Pull upward with steady, even pressure. Do not twist or jerk the tick.
4. If the mouthparts break off and remain in your skin — don't panic. If you cannot easily remove with tweezers, leave it alone and the skin will heal.
5. Clean the bite area and your hands thoroughly with rubbing alcohol, soap or water. Or, even better, take a shower.
6. Dispose of the tick either by putting it in alcohol, wrapping it tightly in tape or flushing it down the toilet.
(Source: Centers for Disease Control and Prevention)
Anyone who spends time outdoors is at risk of encountering ticks. Here's how to take precautions.
1. Avoid areas with high grass.
2. Walk in the center of trails when hiking.
3. Wear long sleeves, long pants and socks when outdoors.
4. Check yourself for ticks on a routine basis, but especially at the end of the day. Using a hand-held or full-length mirror, pay special attention to your scalp, behind your ears, behind your knees, under your arms and in your groin area.
5. Put your dry clothes in a dryer on high heat for 10 minutes after you come indoors. This will kill any ticks.
Should you use bug spray?
You should use only insect repellents registered through the Environmental Protection Agency and only use them as directed. As Ford says, "These are insecticides. More is not always better."
And remember: When wearing repellent or even sunscreen, avoid handling wildlife and swimming in creeks and rivers. Studies have shown that when these chemicals are present in surface waters, they have detrimental effects on salamander and frog populations.
For a chemical-free option, the EPA recommends a repellent made with the oil of lemon eucalyptus.
Did You Know?
Ticks are in the arachnid family, related to scorpions, spiders and mites.
Top reported tick-borne diseases in Tennessee
1. Rocky Mountain spotted fever, 88 cases in 2022
2. Ehrlichiosis, 73 cases in 2022
3. Lyme disease, 30 cases in 2022
(source: Tennessee Department of Health)

