WHAT ARE MESENCHYMAL STEM CELLS?Mesenchymal stem cells, or adult stem cells, are undifferentiated cells found in tissues or organs that can renew themselves and differentiate to yield some or all of the major specialized stem cell types of the tissue or organ.The primary role of adult stem cells is to maintain and repair the tissue in which they are found.Scientists believe MSCs hold some of the greatest promise for wound-healing therapies, because they are so accessible and because they can grow into so many different kinds of cell types.MSCs are already embedded in some FDA-approved wound healing products as a part of a cellular repair matrix.Source: National Institutes of Health; Stem Cell Network; Osiris Therapeutics Inc.
Bobby Rice had a choice to make: Lose his foot. Or take a risk and maybe lose his foot anyway.
He took the chance.
And that choice placed Rice at the center of a could-it-be-true story featuring a small-town doctor and a big-league medical advancement rarely seen at even the most elite hospitals.
Cutting-edge stem cell treatment in Dalton, Ga.?
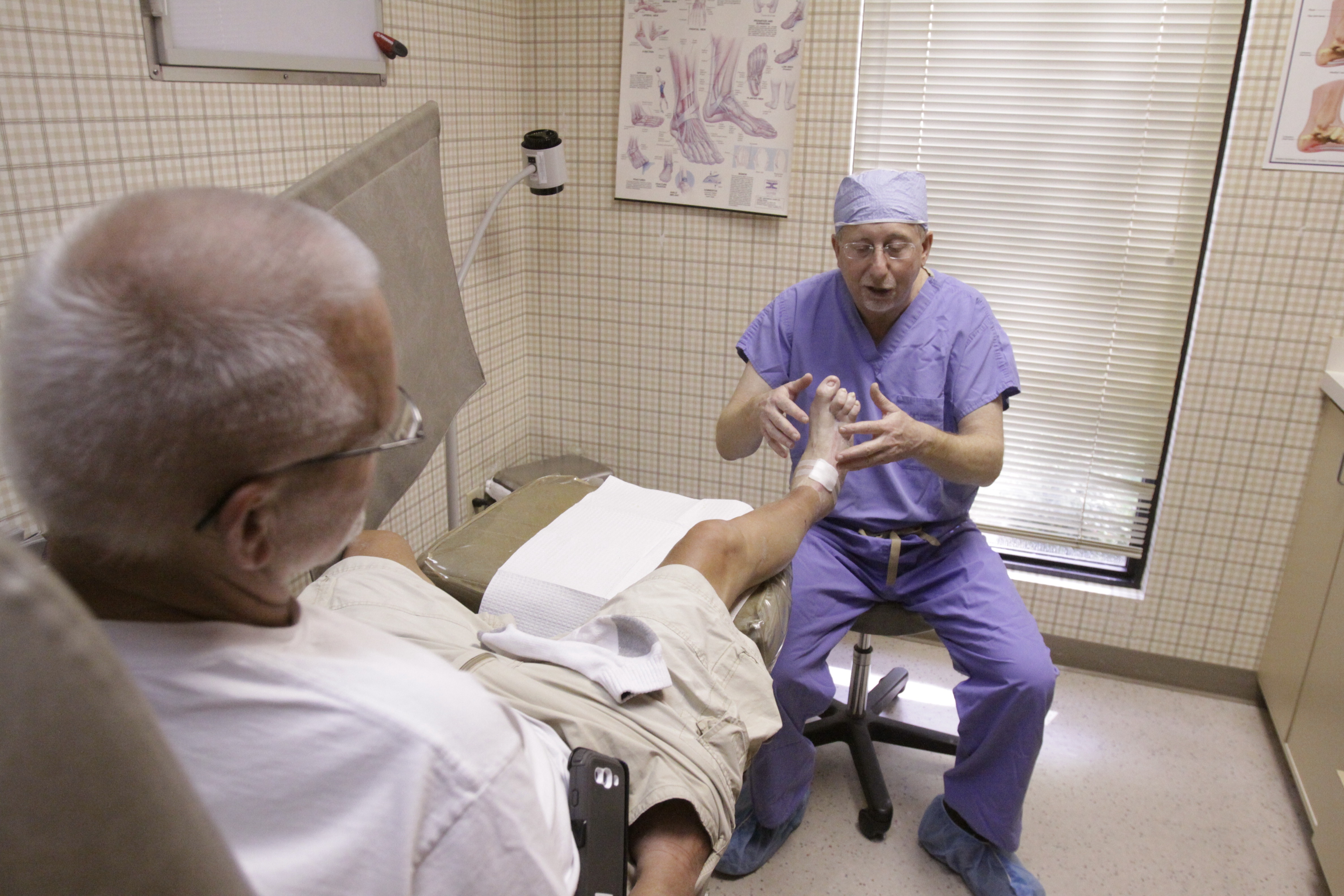
To become a believer, says Dr. Spence Misner, look at the end of Rice's right leg.
The foot looks good these days, Misner, a podiatrist, tells Rice on a recent checkup at the Dalton Foot and Ankle Surgery Center.
It may seem like an insincere compliment. Rice's foot is warped from the flesh-eating infection that ravaged his lower leg. He's missing his baby toe. The skin is puckered. A long, pink scar stretches from his ankle to his toes.
But the foot looks good. For one thing, it's still there.
Supple skin has filled in over the gash. And beneath it is new muscle tissue, new blood vessels, new fat and even new nerve endings.
All thanks to more than $100,000 worth of donated stem cell therapy.
The unlikely story of a gangrenous foot, healed by a doctor who had never worked with stem cell therapy before, has gained a lot of local attention. And medical groups across the country want to know the tale of what's being called The Dalton Foot.
This week, Misner takes the story on the road to a medical conference in Denver. The presentation will be at a gathering of more than 2,000 wound-care specialists.
He acknowledges that it's an odd tale.
"This stuff is not done in a small community hospital. This is done in major university settings," he says. "I'm just a local doctor in a local hospital in a small town."
THE INFECTION
The story of The Dalton Foot starts with a cut.
It didn't seem like an especially bad cut. Rice, 49 at the time, had gotten plenty of nicks and bruises over the years, installing flooring with his brother.
So when he sliced the sole of his foot on a piece of glass one day in fall 2011, he gritted his teeth and bore it.
Days passed. Rice kept changing his socks as fluid from the cut soaked them. Finally fed up, he Superglued his skin shut.
"I've done that for years, being in the flooring business," he quips. "It's always worked."
It was the worst thing he could have done, Misner said later.
The infection quickly festered and swelled. Unknown to Rice, the wound began to contract necrotizing fasciitis -- more popularly known as "flesh-eating bacteria" -- which displayed itself in patches of gangrene and blistering hot skin.
His temperature soared to 103 degrees, and he dipped in and out of consciousness. At one point, his auburn-haired mother, long deceased, appeared before him.
His time hadn't come yet, she told him.
Rice ended up in the emergency room at Hamilton Medical Center in Dalton. Physicians called in Misner, who has specialized in wound care over his 30-year career.
In surgery, Misner snipped away dead and infected flesh and amputated Rice's toe.
His foot lost all feeling.
His tendons were exposed in a gaping, raw gash he describes as something out of "one of the 'Saw' movies."
"It was pretty much a filet," he jokes.
Doctors weren't sure what to do next.
THE TREATMENT
There was little hope the foot would ever recover.
The bacteria had been stopped. But the laceration left behind was too big and too deep for traditional healing methods.
Rice's outlook was further complicated because he had untreated diabetes, and he didn't have medical insurance.
Still, Misner wasn't going to give up on the foot.
For six weeks he tried everything he knew to try. He used a wound vac that applied negative pressure to the wound to stimulate cell growth. He administered intravenous antibiotics. Nothing changed.
Finally, he turned to the owner of a medical supplies company he had worked with for years.
He needed something out of the box, Misner told the businessman. He needed something different, something special. Come see what we're up against, he said.
So Ed Fickey, owner of the Gainesville, Ga.-based medical distribution company Featherbone Medical Inc., came to visit Rice.
The mass of scaly, infected flesh at the bottom of Rice's leg was so dark, Fickey initially thought the patient was wearing a black sock.
If the foot could be saved, they would need some kind of miracle treatment. It turned out Fickey had something that just might work.
A few months earlier he had taken on a new product: Tissue grafts embedded with adult stem cells.
The grafts are tiny squares of placental matrix lined with growth factors, skin-growing cells, connective tissue cells and stem cells.
The stem cells are not taken from human embryos, as many people still assume when they hear the phrase. They are mesenchymal -- adult -- stem cells taken from the placenta after a baby is born.
The cells are exciting to researchers and wound-care specialists because they can grow into a variety of different cell types, including blood vessel and skin cells.
Research and clinical trials of using the cells for wound healing have been going on for more than a decade, experts say.
Several products with these kinds of cell therapies only recently have been approved by the U.S. Food and Drug Administration and have entered the market.
But doctors still are reluctant to use them. Guidelines are being ironed out. Universities and research institutes across the world are investigating the treatment's impact.
Working with such therapies is "certainly not mainstream yet, but it is no longer considered fringe," says Don L. Gibbons, senior science and education communication officer for the California Institute for Regenerative Medicine.
"Most of these early stem cell therapies, however, still need to be refined to figure out the best type of cells to use, the best way to deliver them, and when. For that reason, we urge people to take part in this through registered clinical trials."
Patients are wary of pursuing the treatments because of the unknowns. And the very high costs are not covered by insurance companies.
Each 2-inch by 2-inch sheet of tissue that Fickey proposed using on Rice's foot would cost close to $2,000. Rice would need several dozen.
But Misner and Fickey thought pursuing the treatment was worth a try.
"It made sense for him to try it," Fickey said. "Dr. Misner is a special doctor. He is as good as there is in that field. He had a patient, a product and potential solution."
They appealed to Osiris Therapeutics Inc., which makes the sheets. They presented Rice's predicament and made a case for why he would be a good candidate.
Rice's story intrigued company officials. Their product had been used on a variety of wounds, but none as extensive or complicated as this. But there was a chance the treatment could work.
They agreed to donate the tissue -- eventually committing more than $100,000 worth, Fickey said.
But Rice had to be OK with treading into foreign medical territory.
"I presented it to Bobby and said, 'This has never been done before. I'm not sure it is going to work. But your options are: We amputate your leg now, or we try this, and if it doesn't work, we amputate it later,'" Misner said.
Rice didn't hesitate.
"He was offering me the one chance I'd get," he said. "I didn't mind if it seemed like a big experiment."
THE PROCESS
Misner was committed to healing the foot. But as he looked from it to the new product in his operating room, he wasn't sure where to start.
He had specialized in wound care for more than a decade. He had worked with complex tissue transplants to help heal patients with diabetic ulcerations and other painful wounds.
But he had never worked with stem cells. As he was getting to know the product, he asked company representatives what the protocol would be for someone like Rice.
Their answer? There was no real protocol for someone like Rice. They had guidelines for more specific wounds, but nothing to address the sort of injury and conditions Rice had.
So Misner worked carefully.
The tissue sheets had to be stored at minus-70 degrees in a sterile container, which then had to be quickly thawed and immersed in saline.
Applying the tissues was painstaking. The sheets were nearly impossible to work with. Think of cling wrap, and then imagine it 50 percent thinner. Then picture the extra-thin cling wrap coated with goo, constantly getting twisted as you try to lay it flat.
For weeks, Misner wrestled with the tiny sheets, layering them across the flesh and tendons of the cut. Rice curiously watched him work.
They would document each step of the process, and Fickey would present progress to Osiris.
After three weeks, Misner began to notice changes -- tiny in scale, but mammoth in significance: Red granulation around the tendons. Connective tissue. The cells were turning into ligament, muscle, fat and finally -- skin. The wound was healing.
During one appointment, a nurse tickled Rice's foot. He felt it.
AFTERMATH
Reactions to Rice's treatment and The Dalton Foot are mixed, Misner says.
When he explained the case to other physicians and researchers at a wound conference last year, he was met with head-scratching and surprise. Some doctors thought he was crazy for trying what he tried, he says.
He's not sure how doctors in Denver will react to his presentation.
Since the operation, Misner has gotten calls from patients and physicians across the country who have heard about The Dalton Foot. Some called wanting Misner to operate on them.
He's given advice, but he hasn't tried to take on any more patients like Rice.
The Dalton Foot was a one-shot deal for him. For now, at least. He's not banking on getting a $100,000 donation of stem cells again. And, simply put, stem cells aren't his specialty. More-qualified specialty doctors are the ones to move the treatments into the mainstream, he says.
Dr. Evangelos Badiavas, a professor and researcher in the Interdisciplinary Stem Cell Institute with the University of Miami, says Misner's results are consistent with similar clinical trials he has overseen.
"We've seen return of sensation, vascular growth. We've actually seen prevention in scarring," said Badiavas, who has treated chronic wound patients with bone marrow stem cells for several years.
But he says it's not common for a doctor like Misner to pull this off.
At Erlanger Health System, stem cell therapy isn't being used to heal wounds yet.
"It's slow. I think it will be five to 10 years before we see things that are available and reasonable to use. Cost is a big issue," said Dr. Jimmy Waldrop, a reconstructive surgeon with the Plastic Surgery Group.
Waldrop also said that practices and specialists are more likely to hold out on a revolutionary treatment until it is reviewed by multiple journal publications.
But Badiavas points out that Misner's accomplishment is just as relevant as the work being done at research institutes.
"One of the first reports of HIV was through two community doctors. A lot of times the first observations are made in the community -- there's plenty of smart people outside of universities, probably more," he said.
He's careful to add that Misner likely would have to be under careful regulatory supervision if he was going to try to make stem cells a part of his regular treatment.
Misner acknowledges The Dalton Foot is just a wrinkle in the evolution of stem cell medical applications.
"This is in no way a defined, set protocol. It still has to be fine-tuned, and that will take a few years," he said. "This is just a first step."
Meanwhile, Rice is working on getting his foot up to speed.
Rice can drive now. He can walk longer and longer distances without a walker or cane. He can spend hours walking and wheeling his chair around a track. He's gone from a withered 113 pounds at the time of his hospitalization to 165 pounds.
But things are still tough.
He can't work, though he recently was approved for disability. He still feels pain in his foot. When he lies down at night, it feels tight -- like a "stranglehold." Sometimes he feels what he calls "ghost pain" where his pinky toe used to be.
Walking can be agonizing for his hip, but he is allergic to most pain medications. Every three months or so, he has to buy a new pair of sneakers because the soles of his right-foot shoes are worn down from overcompensating to hold his weight.
Though he was lucky enough to get high-dollar stem cell treatment, he can't pay for regular physical therapy, which Misner says is a big missing piece of the treatment.
And because Rice is considered indigent, even simple fixes -- like a shoe insert to help fill his sneaker -- are nearly impossible to get.
Has it been worth it? The pain and the aggravation and all the unknowns? Would it have been better just to get a prosthesis?
"It's a part of me," Rice answers simply, pointing to his foot. "I can't imagine me without it. You never know how important something is till you almost lose it."
Contact staff writer Kate Harrison at kharrison@times freepress.com or 423-757-6673.