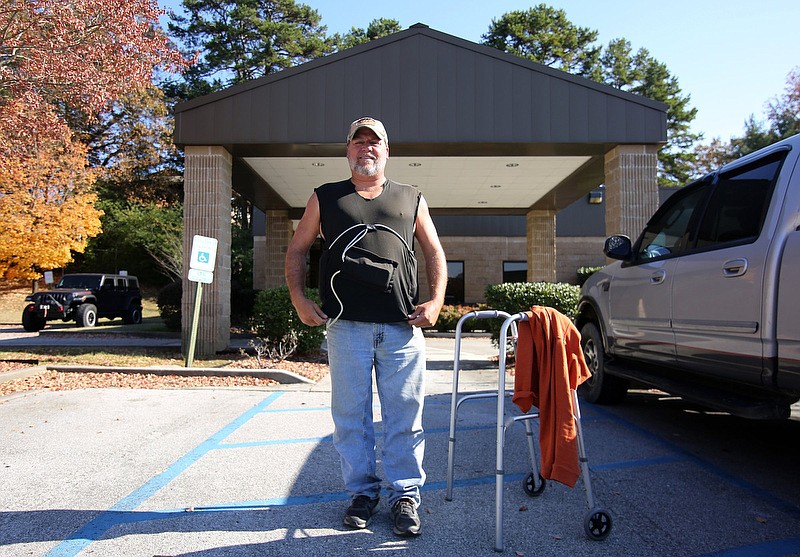
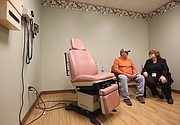
Nurse practitioner Amy Latham placed her stethoscope on Mike Ward's chest during a recent checkup at the Palliative Care Services office in Chattanooga. Instead of the steady rhythm of a beating heart, she heard the humming of a machine.
Ward doesn't have a pulse, but he's very much alive.
A left ventricular assist device pumps blood for his failed heart. The internal pump is used in patients awaiting a heart transplant or in some cases - such as Ward's - when patients need a new heart but aren't candidates for a transplant.
Ward took a chance on the device in 2017. The battery-operated, mechanical pump performs the function of the heart's left ventricle, pumping blood to the rest of the body. And although it's bought him more time, which is important to the single parent, the journey hasn't been easy. Ward said many people living on the device die within the first year.
"I've had it twice that long, and things can happen overnight," he said.
Managing his condition and wondering how much longer his body will hold up can be overwhelming, which is why Ward enrolled in palliative care, a type of specialized medical care that focuses on symptom relief and improving life for people with serious illnesses. Some common conditions that benefit from palliative care include cancer, congestive heart failure, dementia, liver failure and chronic obstructive pulmonary disease, or COPD.
Like many others, Ward had never heard of palliative care and thought it was the same thing as hospice, which also focuses on controlling pain and symptoms but for people who are in their last six months of life. Unlike hospice care, a patient can still seek curative treatments while enrolled in the Palliative Care Services program.
"It's not a place to go die. It's a place to get your quality of life better, but I had not the slightest clue that this even existed," he said.
Ward rarely had a sniffle growing up, but his health began to wane as he approached 40. In his late 30s, he was diagnosed with Crohn's disease. Ward started taking medication, underwent intestinal surgery and began having blood clots in his legs.
He was 40 when his first heart attack struck "out of the blue." He doesn't know much about his family history, but doctors said he was fairly healthy for his age and considering his love of mashed potatoes and gravy. They gave him a stent and prescribed blood thinners to help prevent more clots, but the heart attacks kept coming. Each time, surgeons patched his heart back together.
Ward knew the drill by the time he had his fifth heart attack in August 2017, the day after his 43rd birthday.
He piloted his old Ford F-150 up the driveway toward his house, but this time felt different. He didn't have the usual pain in his ear, jaw, neck and left arm. He started seeing white, tunnel vision. Ward thought maybe he'd gotten too hot and just needed to make it inside, but he never did.
He walked up the stairs and his heart stopped. As he blacked out and fell, Ward's chest landed on a step. He thinks that gave him the jolt he needed to reach for his phone and call 911.
At the hospital, doctors told Ward there was nothing more they could do. He needed a new heart, but liver disease - possibly caused by the years of medications he'd taken to control his Crohn's disease - meant he wasn't a candidate for a transplant.
His family began making funeral preparations as he remained in a hospital bed on life support. He wanted to "take it like a man" and die at home in Rocky Face, Georgia. The plan was to get there, remove the machines and ease his pain with morphine. He'd pass away in a few days, assuming he made it back to Rocky Face.
As he resigned himself to death, a man outside the room asked to speak to Ward. He doesn't remember the man's name, but recalls he was in his mid-70s, wore a white coat and worked in pediatrics at a local hospital.
"He was coming to get a pack of crackers when he overheard them sending a 43-year-old guy home to die," Ward said, adding that the man told him if he wasn't ready to die, "when they come back in, you'll just have to simply tell them, 'If you cant help me, send me somewhere that can.'"
Ward decided he wasn't ready. He was airlifted to Nashville, where he stayed in the intensive care unit for months before finally receiving his left ventricular assist device. At the time, the device hadn't been approved by the U.S. Food and Drug Administration.
"I asked plenty of questions, but there really wasn't a lot of answers other than, 'this can buy you more time,' and really that's all I prayed for - just some more time. I wouldn't say I wasn't spiritually prepared, but I physically wasn't prepared. I had things to do, whether it be more fish to catch, or something," Ward said. "I can tell you, at the end of your life, when it all comes down to just days at any moment, there's nothing you won't give. You'll give up everything you've ever earned, worked for. You'll do anything, and the sad part is, that can't help you in the end - the nicest house and cars, all that stuff, means not one thing. Just another minute with your kid will mean a whole lot more than that."
When it was time to go home, one of the doctors in Nashville recommended that Ward enroll in palliative care. Providers co-manage care with the patient's other doctors to help treat their uncontrolled symptoms, such as nausea, loss of appetite and anxiety, and manage their pain while incorporating emotional, spiritual and social support.
His blood was pumping again, but his life as he knew it was gone. Ward had been an ironworker since his 20s, working on projects like the Chickamauga Dam. That career was now out of the question. He watched his income and most of his social networks disappear as he tried to adjust to his new normal.
"It's scary - to be running literally on batteries, and to try to travel or go to the store by yourself - when you first get that aloneness and nobody's here to help," he said.
Palliative Care Services sees patients in the clinic, in their homes and at hospitals, according to company spokeswoman Mary Danielson. Services are covered by most insurance the same way other medical specialties would be covered, she said. However, lack of awareness and misconceptions often keep people who could benefit from palliative care from seeking help.
"Those range from the falsehood that palliative care is for dying patients to patients having to give up their doctors to receive palliative care," Danielson said. "Unfortunately, the myth that patients have to give up their doctors is also prevalent among doctors who think they have to give up their patients. In reality, we co-manage care with their doctors."
Ward's monthly palliative care appointments last about an hour. His multidisciplinary team of providers - which include physicians, nurse practitioners and social workers - make sure his symptoms are controlled and help him navigate his multiple medical conditions.
For example, with everything else going on, Ward was neglecting his psoriasis - a condition in which skin cells build up and form scaly, itchy, dry patches. His care team noticed the psoriasis inching closer to hole in his side where the heart pump is inserted. Now, Ward is seeing a dermatologist.
"We're holistically looking at the patient and filling in the gaps wherever we can to treat him, because we're more than the physical parts we're built of," Danielson said.
The palliative care team helps by communicating with other providers and coordinating care. They also offer support services to caregivers, since they are often the ones providing direct patient care day in and day out.
"They're not really treating my disease. They're treating my symptoms," Ward said. "Sometimes that can be having a goal for myself and them helping me to achieve it by encouragement. I'm not gonna get that at my heart doctor. He's not going to ask me, are you living on your own again? It's just not his priority, and that's their priority here."
Ward was doing well until hitting another major setback the day after Thanksgiving last year, when he was driving and lost consciousness, crashing head-on into a tree. When he didn't show up for his appointment, Ward's palliative care team went looking for him.
"What people that manage your health call around trying to find you if you don't show up, besides trying to collect your money, you know?" he said.
These days, Ward is fishing more and living on his own again - two major goals he says he accomplished thanks to his care team. They've also discussed the possibility of finding the man in the white coat from the hospital.
"It took God and sending that little man to get a pack of crackers to get me to where I'm at. I wouldn't be here. I wouldn't get to see my son graduate and walk across the stages at the Army. It's just all stuff that I value very highly," Ward said. "They can't heal me. I know this. But I can have a better quality of life because of them, this place, palliative care."
Contact Elizabeth Fite at efite@timesfreepress.com or 423-757-6673.