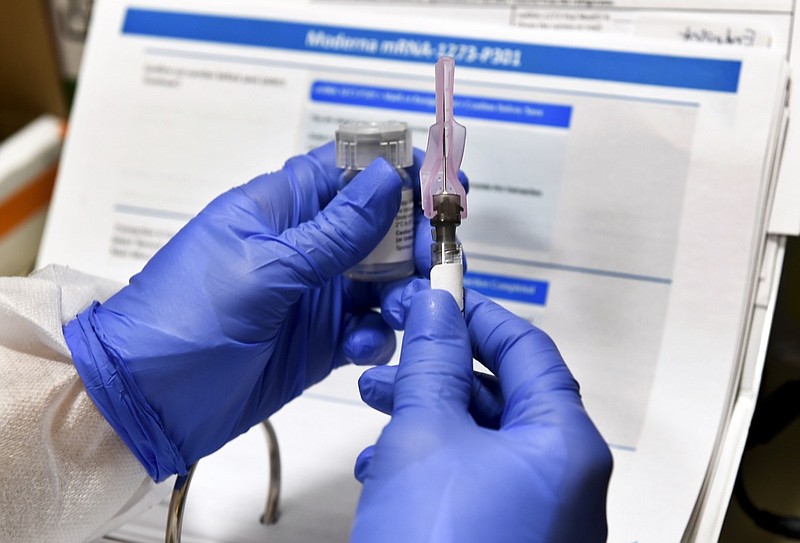
More than 100 vaccines to address the COVID-19 pandemic are in various stages of development. Five candidates have received funding from the U.S. government under Operation Warp Speed, which aims to make 300 million doses of a safe, effective vaccine available for the U.S. market by January 2021. In the past, the development of a new vaccine typically required years for research and testing.
A new vaccine is first administered to animals to determine if an antibody response is produced. If so, the vaccine is tested in human subjects in three phases.
Phase 1 involves giving the vaccine to a small group of healthy volunteers to ascertain safety, determine acceptable side effects, and establish the minimum dose necessary to produce an antibody response. Fever and muscle aches were experienced in subjects who received higher doses of COVID-19 vaccine in recent phase 1 trials.
Phase 2 extends the trial to several hundred volunteers across the age spectrum and includes individuals with chronic health conditions, such as diabetes, obesity and asthma. Subjects are recruited from diverse racial and ethnic backgrounds. Safety and effectiveness are closely monitored.
Phase 3 is a "blinded study." Subjects are randomly assigned to receive vaccine or a placebo (an inactive material). Neither the subject nor the clinic administering the injection knows if vaccine or placebo is injected in a subject. For this phase, 30,000 subjects will be tested at multiple locations where active outbreaks of COVID-19 are underway. Two injections will be given four weeks apart to each participant. Subjects will be closely followed to determine if the vaccine prevents COVID-19 infection. Side effects will be recorded in both groups. The period of observation will extend for months. Results are continuously monitored at a central site. A vaccine is judged effective if it reduces infections by at least 50%. A trial could be ended if dangerous, unexpected side effects are observed.
Phase 3 trials have begun for two vaccines.
After intensive review of experimental data, the U.S. Food and Drug Administration grants final approval to a vaccine. The agency inspects production facilities and requires testing for purity of each lot of vaccine before its shipment. A waiver can be granted by the FDA for emergency use of a vaccine.
Once an effective vaccine is available in the U.S., it will be administered at no cost to the recipient.
A successful licensee will need to produce tens of millions of doses rapidly to meet national needs for the initial injection and the follow-up booster. A like number of glass vials will be required along with syringes and other equipment such as refrigeration. Another challenge will be establishment of sufficient numbers of sites across the country for safe vaccination of large numbers of people.
Particularly in the year of a presidential election, political pressure must be avoided in rushing a vaccine to market before adequate testing for effectiveness and safety has been completed.
Polling reported in Science magazine in June indicates that 50% of adults do not plan to take a COVID-19 vaccine, while an additional 25% are unsure.
Several questions persist: Will an annual booster vaccination be required to maintain immunity? If multiple vaccines successfully complete testing, will each be approved? If the first successful vaccine is developed in one country, will its administration be limited to residents of that country or will the vaccine be distributed internationally? Who will determine priorities for receiving a vaccine once it is approved? Could schools require vaccination of all students? Could a nation require evidence of vaccination before admitting a traveler? Could governmental offices, legislative bodies and businesses require vaccination? What agency will oversee and fund international distribution of a vaccine, especially in Third World countries?
In the most favorable circumstances, years may be required to control COVID-19.
Contact Clif Cleaveland at ccleaveland@timesfreepress.com.